2023 年 23 巻 1 号 p. 9-13
2023 年 23 巻 1 号 p. 9-13
Indirect composite restorations made of highly loaded light and heat polymerized material were applied to the mandibular premolars of a 23-year-old female patient. Enamel cavity margins were etched with phosphoric acid. Dentin surfaces to be bonded were treated with ferric chloride-citric acid solution, and coated with tri-n-butylborane (TBB)-initiated 4-META resin. Inner surfaces of the inlays were treated with phosphoric acid. The restorations were then seated with dual-polymerized composite luting agents. Although cavosurface discoloration, wear, loss of marginal integrity, and change in surface texture were detected, both restorations are still functioning after 33 years. Restorations made with such system is applicable for premolar class II cavities and have a favorable prognosis.
Composite restorations have generally been applied for class I, III, IV, and V cavities. Development of varied composite material has shown that they can be used for class II restorations. Both direct and indirect composite materials with different initiation modes are currently available. Indirect composite resin systems initiated with heat, light, or dual mode are applicable in the fabrication of inlay and onlay restorations as well as composite resin veneered metallic restorations.
Light and heat polymerized indirect composite resin is used for class II premolar restorations. One of the advantages of indirect restoration is the reliable recovery of anatomic form for proximal molar surfaces. In addition, intraoral construction of distal anatomic form with direct composite material requires considerable skill, especially in the cervical area. Although comparisons between direct and indirect composite restorations have been extensively reported, limited information is available about the long-term clinical performance of indirect composite restorations [1,2]. This case report describes the long-term clinical performance of premolar composite inlay restorations bonded with 4-META [3,4,5]-Mac 10 [4,5,6] adhesive system. Modified USPHS criteria [7,8] was used in evaluation of the clinical course of restorations.
A 23-year-old woman was seen with the chief complaints of esthetic and masticatory disturbance derived from the appearance of a metallic premolar restoration as well as cold water pain of the first premolar. Examination revealed secondary dental caries around the distal cervical area of the second premolar, whereas dental caries was seen across the distal dentino-enamel junction of the first premolar. The patient preferred a tooth-colored restoration rather than a metallic restoration. The dental surgeon, however, did not consider that a direct composite resin restoration was applicable in this case. This was based on the fact that cavity preparation would be extended for both teeth from occlusal surface to entire distal surface.
Several treatment options were proposed, and the patient preferred either indirect composite resin restoration or porcelain inlay restoration. After written consent was obtained, both premolars were restored with indirect composite resin restorations, and seated with 4-META-MAC 10 combined adhesive system.
Clinical and laboratory procedureMaterials used in this case are summarized in Table 1. Cavities with rounded line angle and point angle were prepared with a diamond rotary cutting instrument (102R, 201, 301, 364R, Shofu Inc., Kyoto, Japan). An impression was made with a silicone elastomeric material (Exaflex, GC Corp., Tokyo, Japan) and poured with die stone. Inlay restorations were fabricated with a highly loaded composite material (Palfique Inlay, Tokuyama Soda Inc., Tokyo, Japan). The restorations were light-exposed for 90 s with a xenon light source (Dentacolor XS, Kulzer & Co., GmbH, Friedlichsdorf, Germany), and secondarily polymerized for 20 minutes at 100˚C with a heat oven (TP-1000, Tokuyama Soda Inc.).
Table 1 Materials employed
| Material | Trade name | Composition |
|---|---|---|
| Indirect composite | Palfique Inlay | 85% filler, splintered silica-zirconia, spherical quartz (2-3 µm), di-methacrylate |
| Adhesive | Super-Bond D-Liner | 4-META, HEMA, MMA, di-methacrylate, TBB |
| Luting agent | Palfique Inlay Cement | MAC-10, spherical silica-zirconia, di-methacrylate |
HEMA, 2-hydroxyethyl methacrylate; MAC-10, 11-methacryloyloxy-1,1-undecane dicarboxylic acid; 4-META, 4-methacryloyloxyethyl trimellitate anhydride; MMA, methyl methacrylate; TBB, tri- n -butylborane derivative
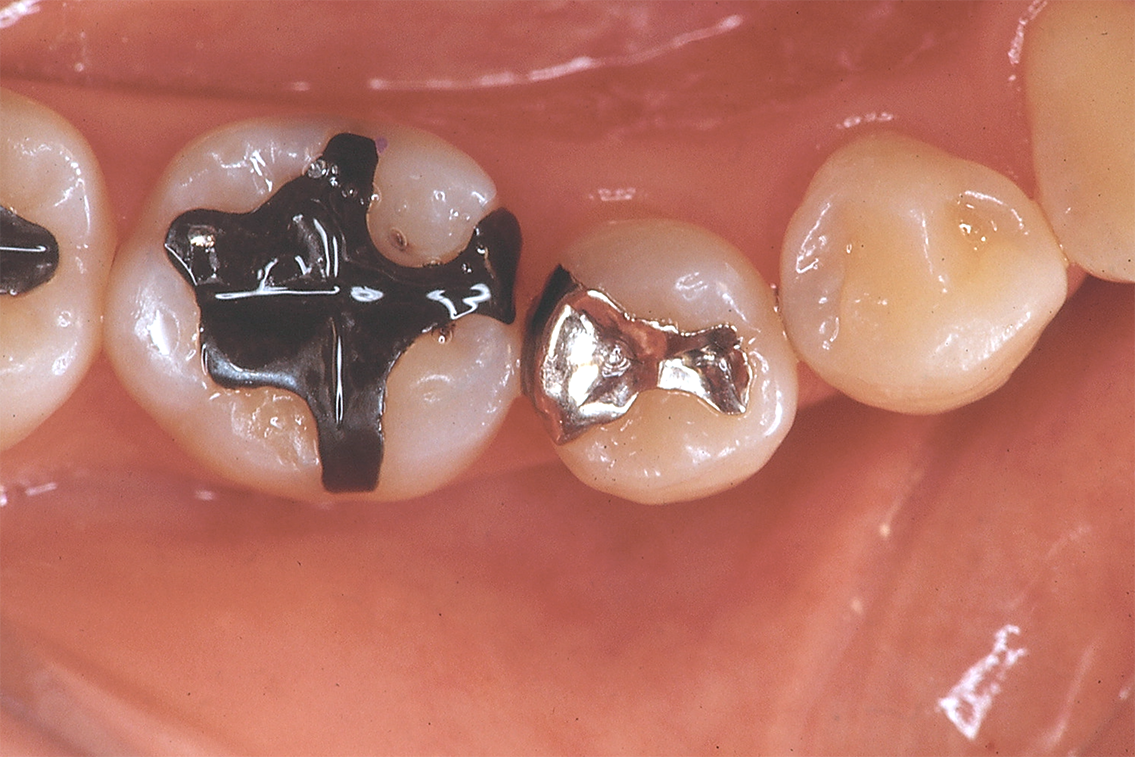
Fig. 1 Preoperative view of premolars
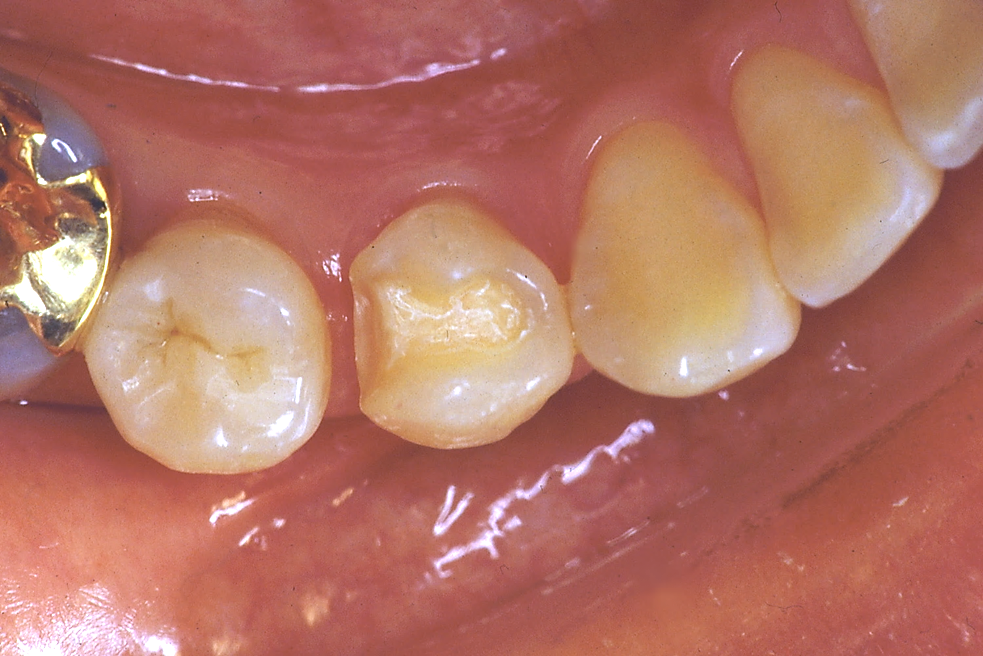
Fig. 2 Class II cavity preparation for the first premolar

Fig. 3 Seated indirect composite restorations

Fig. 4 Occlusal view 10 years after seating
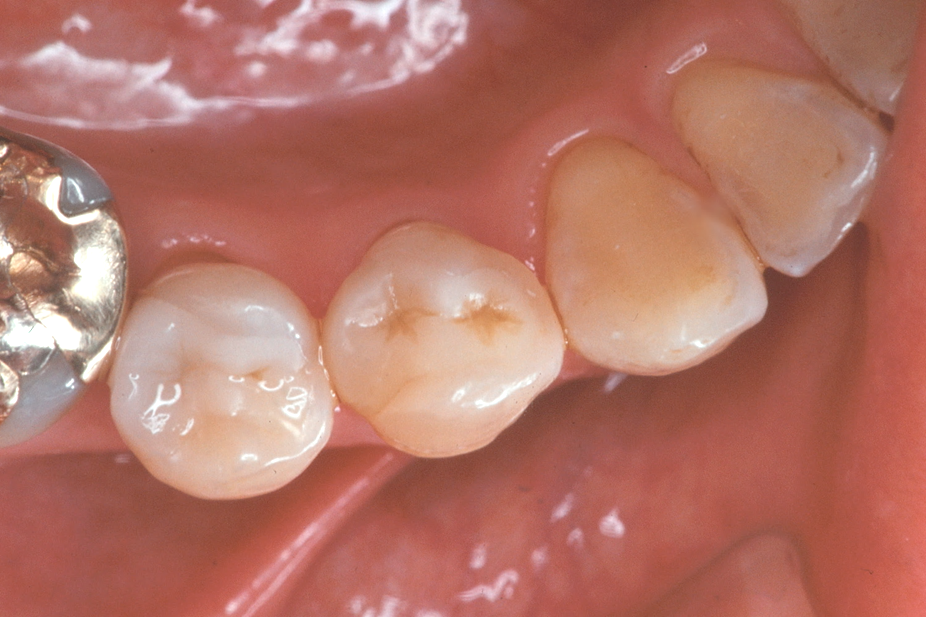
Fig. 5 Occlusal view 13 years after seating

Fig. 6 Occlusal view 22 years after seating
At the patient’s next visit, the restorations were tried-in, and the surface to be bonded was cleaned with phosphoric acid gel, ultrasonically cleaned in a water-bath, and air-dried. Marginal enamel surfaces of cavity preparation were etched with 38% phosphoric acid gel (Tokuyama Soda Inc.) for 20 s, whereas dentin surfaces of the cavity floor, axial wall, and flair were treated with 10% citric acid-3% ferric chloride (Sun Medical Co., Ltd., Moriyama, Japan) for 10 s, washed with
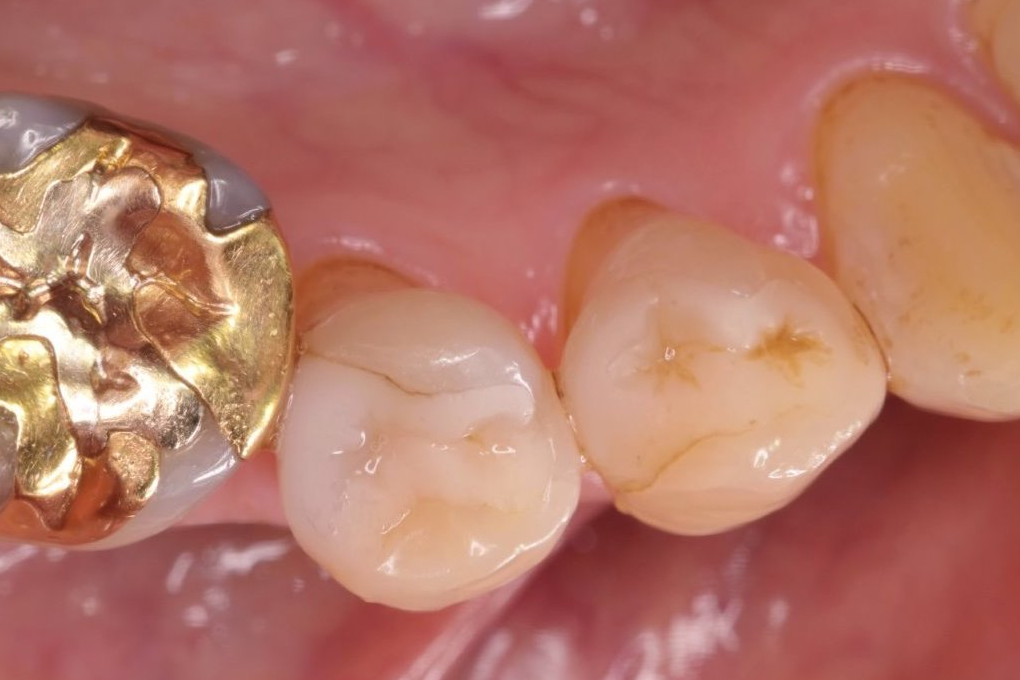
Fig. 7 Occlusal view 27 years after seating
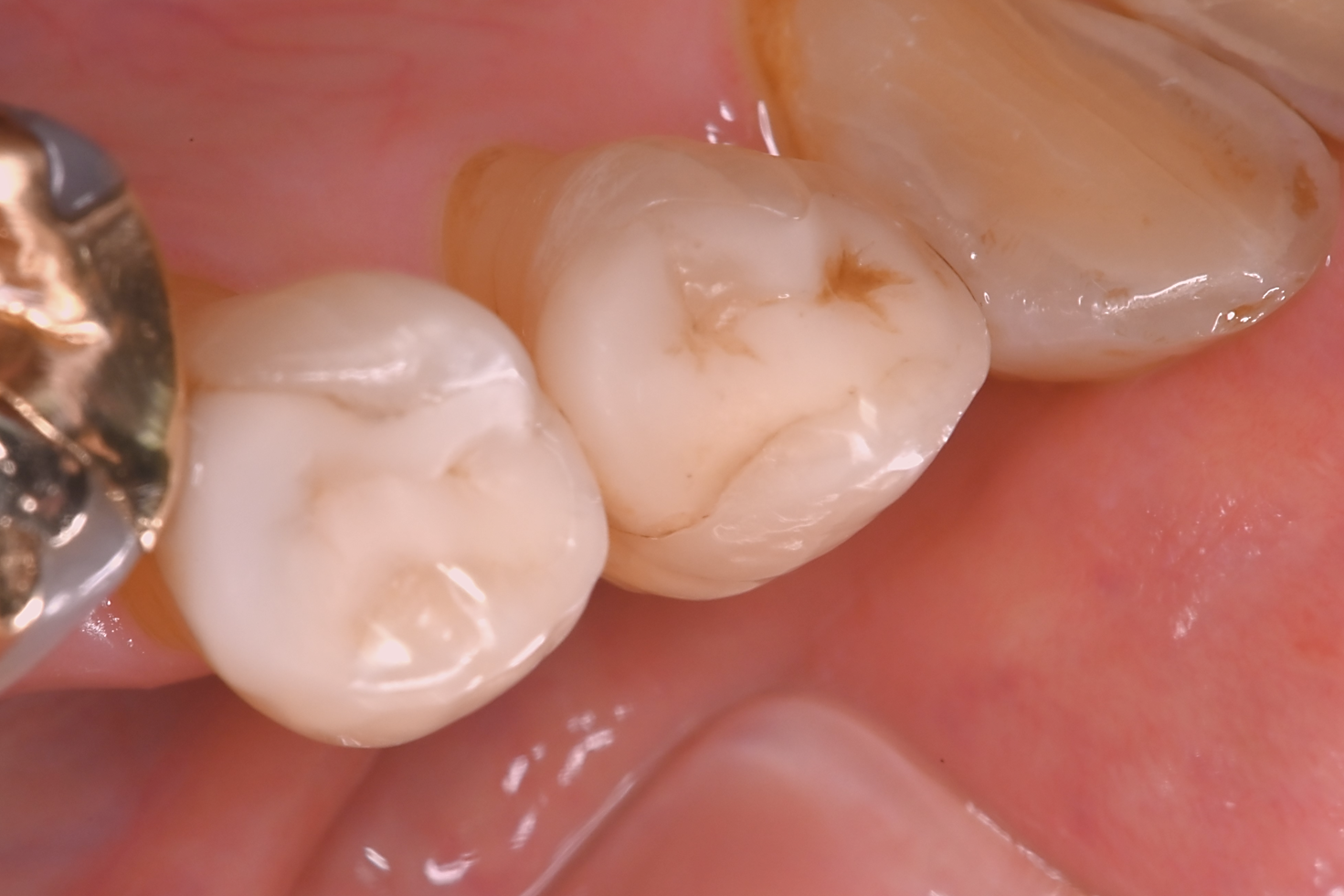
Fig. 8 Occlusal view 33 years after seating
Table 2 Modified USPHS criteria for direct evaluation of composite restorations
| Color match | Alfa (A) | There is no visual evidence of marginal discoloration different from the color of the restorative material and from the color of the adjacent tooth structure. |
|---|---|---|
| Bravo (B) | The restoration does not match the shade and translucency of adjacent tooth tissues, but the mismatch is within the normal range of tooth shades. | |
| Charlie (C) | The restoration does not match the shade and translucency of adjacent tooth structure, and the mismatch is outside the normal range of tooth shades and translucency. | |
| Cavosurface marginal discoloration | Alfa (A) | There is no visual evidence of marginal discoloration different from the color of the restorative material and from the color of the adjacent tooth structure. |
| Bravo (B) | There is a visual evidence of marginal discoloration at the junction of the tooth structure and the restoration, but the discoloration has not penetrated along the restoration in pulpal direction. | |
| Charlie (C) | There is a visual evidence of marginal discoloration at the junction of the tooth structure and the restoration that has penetrated along the restoration in a pulpal direction. | |
| Recurrent caries | Alfa (A) | The restoration is a continuation of existing anatomic adjacent to the restoration. |
| Charlie (C) | There is visual evidence of dark deep discoloration adjacent to the restoration. | |
| Wear | Alfa (A) | The restoration is a continuation of existing anatomic form or is slightly flattened. |
| Bravo (B) | A surface concavity is evident. | |
| Charlie (C) | There is a loss of restorative substance such that a surface concavity in evident and the base and/or dentin is exposed. | |
| Marginal integrity | Alfa (A) | The explorer does not catch when drawn across the surface of the restoration toward the tooth, or, if the explorer does catch, there is no visible crevice along the periphery of the restoration. |
| Bravo (B) | The explorer catches and there is visible evidence of a crevice, into which the explorer penetrates, indicating that the edge of the restoration does not adapt closely to the tooth structure. | |
| Charlie (C) | The explorer penetrates crevice defect extended to dentinoenamel junction. | |
| Surface texture | Alfa (A) | Surface texture similar to polished enamel as determined by means of a sharp explorer. |
| Bravo (B) | Surface texture gritty of similar to a surface subject to a white stone or similar to a composite containing supramicron sizes particles. | |
| Charlie (C) | Surface pitting is sufficiently coarse to inhibit the continuous movement of an explorer across the surface. |
water, and air-dried. A tri- n -butyl borane (TBB)-initiated adhesive (Super Bond D-liner, Sun Medical) was applied to the cavity preparations, and both inlay restorations were seated with dual-polymerized luting composite that contains carboxylic functional monomer MAC-10 (Palfique Inlay Cement, Tokuyama Corp.). After minimal light exposure, excess material was removed and the luting composite was light-exposed from four directions with a 30 s interval. Occlusion and articulation were adjusted, and the surfaces were finally polished with diamond paste using a rotary polishing instrument. The patient then entered the observation procedure.
Clinical courseBoth restorations were observed every year by means of the modified USPHS criteria (Table 2) [7,8]. Table 3 summarizes the evaluation up to 33 years of the two restorations. During the observation period, loss of color match, cavosurface marginal discoloration, wear, deterioration of marginal integrity, and change in surface texture were detected. Both restorations, however, have been functioning satisfactorily for more than 30 years.
Table 3 Evaluation of indirect composite restorations from the base line to 33 years after seating
| Criteria | Restoration | Observation period (years) | ||||||
|---|---|---|---|---|---|---|---|---|
| BL | 5-y | 10-y | 13-y | 22-y | 27-y | 33-y | ||
| Color Match | 44 | A | A | A | A | B | B | B |
| 45 | A | A | A | A | B | B | B | |
| Cavosurface marginal discoloration | 44 | A | A | A | A | B | B | C |
| 45 | A | A | A | A | B | B | B | |
| Recurrent caries | 44 | A | A | A | A | A | A | A |
| 45 | A | A | A | A | A | A | A | |
| Wear | 44 | A | A | A | A | A | B | B |
| 45 | A | A | A | A | A | A | B | |
| Marginal integrity | 44 | A | A | A | A | B | B | B |
| 45 | A | A | A | A | B | B | B | |
| Surface texture | 44 | A | A | A | A | A | A | B |
| 45 | A | A | A | A | A | A | B | |
The authors applied the D-Liner 4-META adhesive system to the dentin portion of prepared cavities. Neither of the premolars showed any symptoms of pulp irritation over a period of 30 years. These results may derive from the application of ferric chloride together with TBB-initiated 4-META resin, which is reported to be useful as a pulp capping material [9]. However, both of the restorations exhibited cavosurface marginal discoloration after 20 years or more. The authors consider that discoloration originates in part from the formation of a complex compound between amine reducing agent in the luting composite and 4-META carboxylic anhydride monomer in the adhesive agent [10]. Care should be taken in the application of 4-META adhesive resin together with composite luting agent initiated with peroxide-amine, or quinone-amine redox system. Application of 4-META acrylic adhesive should be avoided in the cavosurface marginal area to prevent marginal discoloration and wear of luting agent.
Wear and change in surface texture were not remarkable in either of the restorations. This result may derive from the increased filler loading (85%) and application of fine spherical particles with 2-3 µm diameter of the indirect composite material.
One of the issues associated with indirect composite resin system is that an ideal adhesive system for thermosetting composite resins has yet to be developed. This fact hinders the application to laminate veneers of thermosetting composites such as prefabricated CAD-CAM block.
MN: conceptualization, investigation, methodology, validation, investigation, resources, data curation, writing original draft. HH: conceptualization, methodology, supervision, formal analysis, writing, review and editing. All authors read and approved the final version of the manuscript.
The authors declared no potential conflicts of interest with respect to this report, authorship, and/or publication of this article.
All data generated or analyzed during the current study are available from the corresponding author on reasonable request.
Summary of clinical and laboratory procedure has been presented in the following publications. The authors thank Hyoron Publishers, Tokyo, Japan, for permission of re-use of the materials presented in the current report (Figs. 2, 3, and 5). Figures 2 and 3: Nakamura M. Technical method and clinical result of a composite resin inlay restoration. Nippon Dent Rev 1990; 576: 119-33. Figure 5: Nakamura M. Long-term assessment of composite resin inlay restorations. Nippon Dent Rev 2003; Separate vol.: 123-9.