Abstract
Background:
Door-to-balloon (DTB) time ≤90 min is an important quality indicator in the management of ST-elevation myocardial infarction (STEMI), but a considerable number of patients still do not meet this goal, particularly in countries outside the USA and Europe.
Methods and Results:
We analyzed 2,428 STEMI patients who underwent primary PCI ≤12 h of symptom onset who were registered in an ongoing prospective multicenter database (JCD-KiCS registry), between 2008 and 2013. We analyzed both the time trend in DTB time within this cohort in the registry, and independent predictors of delayed DTB time >90 min. Median DTB time was 90 min (IQR, 68–115 min) during the study period and there were no significant changes with year. Predictors for delay in DTB time included peripheral artery disease, prior revascularization, off-hour arrival, age >75 years, heart failure at arrival, and use of IABP or VA-ECMO. Notably, high-volume PCI-capable institutions (PCI ≥200/year) were more adept at achieving shorter DTB time compared with low-volume institutions (PCI <200/year).
Conclusions:
Half of the present STEMI patients did not achieve DTB time ≤90 min. Targeting the elderly and patients with multiple comorbidities, and PCI performed in off-hours may aid in its improvement.
Primary percutaneous coronary intervention (PCI) is a life-saving treatment for ST-segment elevation myocardial infarction (STEMI),1–3
and, importantly over the last decade, shorter patient-specific door-to-balloon (DTB) time, which is the time interval from arrival at hospital to inflation of the balloon to restore coronary flow, is consistently associated with lower long-term mortality.4,5
Consequently, clinical guidelines recommend DTB time ≤90 min,6,7
and this is considered a key indicator for providing high-quality care in the USA.8,9
Studies from large-scale databases have identified predictors and strategies to allow individual hospitals and larger health-care systems to decrease DTB time.10–14
Based on these findings, DTB time has been successfully reduced in Western countries. These implications from Western countries, however, may be limited,15
because of significant differences in patient characteristics16
and PCI-capable facilities,17
and therefore different strategies may be required in non-Western countries, including Japan. Specifically, several studies have emphasized the volume-outcome relationship in the assessment of DTB time, but this trend may differ in universal health care.18
Japan implemented social health insurance in 1961, and, consequently, primary PCI is performed far more aggressively compared with Western countries.16
Hence, to assess country-specific gaps and identify areas for improvement, the aim of this study was to evaluate the current status of STEMI care with regard to DTB time in Japan, and further explore predictors associated with delay in DTB time using a large-scale, multicenter PCI registry.
Methods
Data
We obtained data from the Japan Cardiovascular Database-Keio interhospital Cardiovascular Studies (JCD-KiCS) registry. The JCD-KiCS registry is a prospective registry designed to collect clinical variables and outcome data on consecutive PCI patients, with dedicated clinical research coordinators assigned to each site. Approximately 200 variables were collected from each patient. The JCD-KiCS registry includes 15 institutes within the metropolitan Tokyo area, consisting of mostly large tertiary care referral centers (≥200 beds; n=13), but also includes a few midsized satellite hospitals (<200 beds; n=2). Participating hospitals were instructed to record and register data from consecutive hospital visits for PCI using an Internet-based data collection system. All PCI performed with any commercially available coronary devices were included. The data entered were checked for completeness and internal consistency. Data quality assurance was achieved through automatic system validation and reporting of data completeness, education, and training by clinical research coordinators specifically trained for the present PCI registry. The senior study coordinator (I.U.) and exclusive on-site auditing by investigators (S.K. and H.M.) ensured proper registration of each patient.
The study protocol was approved by the Institutional Review Board committee of each hospital in Japan. All participants provided written informed consent for the study. Before the launch of the JCD registry, information on the objectives of the study and its social significance, and an abstract were provided for clinical trial registration with the University Hospital Medical Information Network. This Network is recognized by the International Committee of Medical Journal Editors as an acceptable registry according to a statement issued in September 2004 (UMIN 000004736).
Subjects and Variables
The present study was analyzed using a dataset of STEMI patients who had undergone primary PCI at ≤12 h of symptom onset between October 2008 and December 2013 (n=2,428). We excluded 88 patients (3.6%) with missing DTB time and 57 (2.3%) with DTB time >240 min to focus on patients who would benefit the most from myocardial salvage (Figure 1).
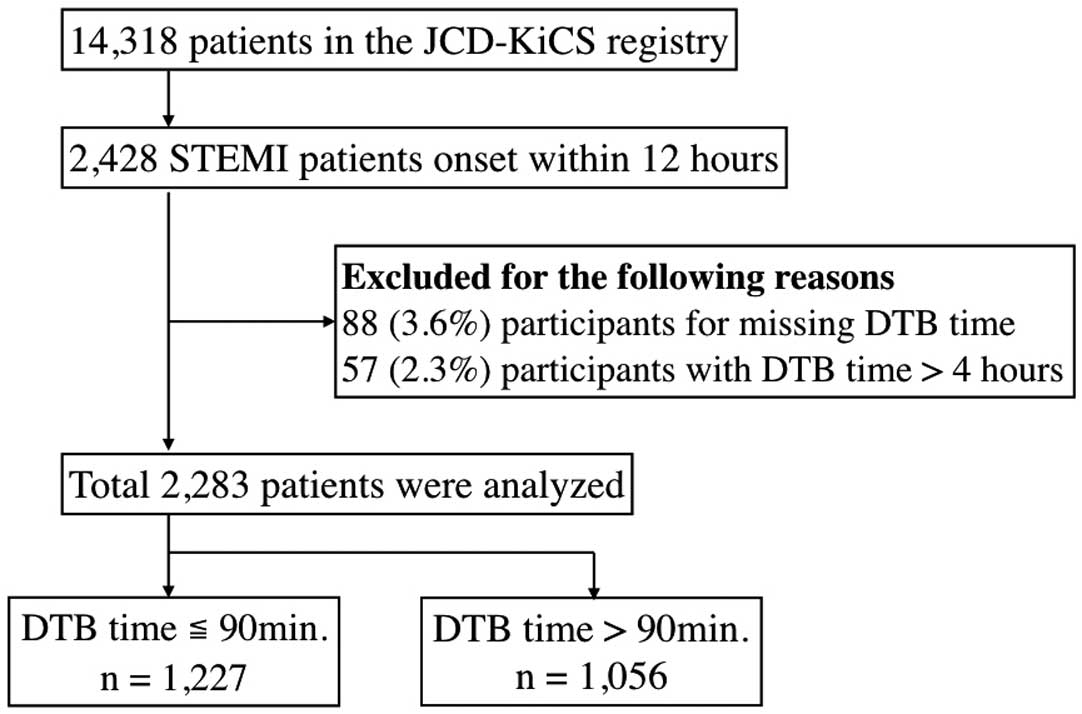
STEMI was defined in accordance with the associated guidelines.6,7
Patient-specific DTB time was based on data from catheterization laboratory visits and defined as the time from initial arrival at a PCI facility to first device use for the culprit artery during primary PCI (e.g., balloon inflation or aspiration thrombectomy). Referral was defined as initial diagnosis at a satellite clinic prior to transport to the second or territorial hospital. Off-hour was defined as arrival between 6 p.m. and 8 a.m on weekdays, or at any time on weekends or public holidays. The remaining clinical variables and in-hospital outcomes of the JCD-KiCS registry were defined in accordance with the national cardiovascular data registry (NCDR) version 4.1.4,19
Specifically, presence or absence of heart failure symptoms and its classification (at the time of arrival) was defined according to the documentation of the attending physician. Peripheral artery disease (PAD) was defined as history of PAD including upper and lower extremity, renal, mesenteric, and abdominal aortic systems. Intra-aortic balloon pump (IABP) use was defined as requirement at the start of or during the procedure.
The primary outcomes of this analysis were temporal trends in annual DTB times and in-hospital mortality (defined as the rate of all-cause death). Annual DTB time was defined as the median of patient-specific DTB times during the year in which the procedure was done in the primary PCI group. We also classified hospitals according to annual PCI volume: median annual PCI volume was 258/year (IQR, 185–353/year), therefore high volume was defined as annual PCI volume ≥200, while low volume was defined as annual PCI volume <200, based on the Japanese Association of Cardiovascular Intervention and Therapeutics.20
Statistical Analysis
The patients were divided into 2 DTB time groups: ≤90 min and >90 min, and the patient and procedure characteristics, as well as hospital care system, comparied. Continuous variables are presented as mean±SD or median (IQR), and categorical variables as numbers and percentages. We compared categorical variables using chi-squared test when appropriate; otherwise, we used Fisher’s exact test. We compared continuous variables with Student’s t-test or Wilcoxon rank-sum test based on the distribution.
Multivariable analysis was used to investigate the independent predictors of DTB time delay. Logistic regression model was constructed by adjusting for clinically relevant variables, and factors that were significantly different between 2 groups (P<0.1) were included in the multivariate analysis. Continuous variables such as age or body mass index (BMI) were dichotomized according to clinical reference values. Factors evaluated in the multivariate model were gender, age >75 years, BMI >30 kg/m2, hypertension, diabetes mellitus, chronic kidney disease (CKD; estimated glomerular filtration rate <60 mL/min/1.73 m2) or hemodialysis, PAD, prior revascularizations, heart failure at arrival, cardiogenic shock at arrival, cardiopulmonary arrest, referral from local clinic, PCI at high-volume centers, off-hour arrival, use of IABP or veno-arterial extracorporeal membrane oxygenation (VA-ECMO), left anterior descending (LAD) lesion, and type C lesion. We tested for an interaction between time of presentation and volume of PCI at the institution, and expected any association between time of presentation and delay to be attenuated at high-volume institutions. The first author used SPSS ver. 23.0 to do all analyses. All reported P-values are 2 sided. P<0.05 was set as statistically significant.
Results
Overall Trend in DTB Time and Mortality
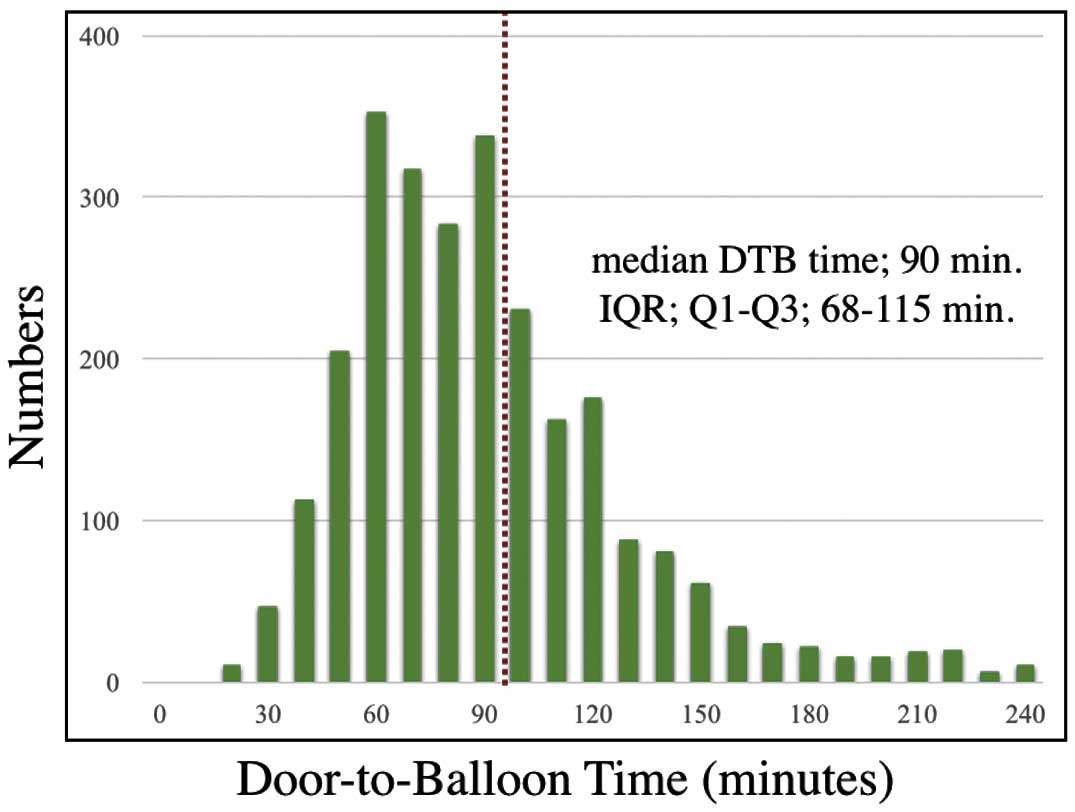
Median DTB time was 90 min (minimum, 22 min; IQR, 68–115 min), with 46.2% of patients having DTB time >90 min (Figure 2); annual trend is given in
Table 1. The median DTB time was slightly increased from 85 min (IQR, 60–120 min) in 2008–2009 to 90 min (IQR, 67–116 min) in 2013, but there was no significant difference (P=0.61). In addition, there was no remarkable change in in-hospital mortality rate during the study period (P=0.67).
Table 1.
DTB Time and In-Hospital Mortality: Annual Trend
| |
2008–2009 |
2010 |
2011 |
2012 |
2013 |
Overall |
| Participating patients |
259 |
442 |
536 |
522 |
524 |
2,283 |
| Participating patients in high-volume centers |
214 (82.6) |
351 (79.4) |
443 (82.6) |
451 (86.3) |
487 (92.9) |
1,946 (85.2) |
| Participating hospitals |
7 |
13 |
13 |
13 |
11 |
15 |
| No. low-volume centers |
3 |
6 |
5 |
5 |
3 |
6 |
| DTB (min) |
85 (60–120) |
88 (67–110) |
90 (70–120) |
90 (70–114) |
90 (67–116) |
90 (68–115) |
| In-hospital death |
16 (6.2) |
27 (6.1) |
33 (6.2) |
37 (7.1) |
28 (5.3) |
141 (6.2) |
Data given as n (%) or median (IQR). DTB, door-to-balloon.
The patients were divided into 2 groups according to DTB time: the 1,227 patients (53.7%) with DTB time ≤90 min were defined as the shorter DTB time group, and the 1,056 patients (46.2%) with DTB time >90 min were defined as the longer DTB time group (Table 2). Patients with PAD were more likely to have longer DTB time (2.3% in shorter DTB time group vs. 4.9% in longer DTB time group, P=0.001). In addition, patients with CKD, prior myocardial infarction (MI), and prior revascularization were more likely to have longer DTB time (P<0.01 for all). In contrast, patients who underwent PCI at a high-volume center (89.8% vs. 79.9%, P<0.001), and who were referred from satellite clinics (26.3% vs. 15.6%, P<0.001) had shorter DTB times. With regards to procedure characteristics, LAD lesion was more common in the short DTB time group (48.3% vs. 41.8%, P=0.002), and IABP (17.2% vs. 23.2%, P<0.001), and left circumflex lesion (8.1% vs. 11.2%, P=0.012) were more common in the longer DTB time group.
Table 2.
Baseline and Procedure Characteristics
| |
DTB time ≤90 min
(n=1,227) |
DTB time >90 min
(n=1,056) |
P value |
| Age (years) |
64.7±12.3 |
66.7±12.8 |
0.18 |
| Male |
971 (79.7) |
807 (77.4) |
0.19 |
| BMI (kg/m2) |
24.0±3.8 |
23.9±3.8 |
0.68 |
| Family history of CAD |
162 (13.1) |
126 (11.7) |
0.29 |
| Past medical history |
| Hypertension |
770 (63.3) |
679 (65.3) |
0.33 |
| Diabetes mellitus |
359 (29.8) |
328 (31.9) |
0.28 |
| Dyslipidemia |
688 (56.6) |
584 (56.2) |
0.82 |
| CKD (eGFR <60 mL/min/1.73 m2) |
356 (31.1) |
384 (39.2) |
<0.001 |
| CKD on HD |
8 (0.7) |
13 (1.3) |
0.14 |
| Peripheral artery disease |
28 (2.3) |
51 (4.9) |
0.001 |
| Prior MI |
94 (7.7) |
118 (11.3) |
0.003 |
| Prior revascularization |
89 (7.3) |
140 (13.3) |
<0.001 |
| Prior PCI |
85 (7.0) |
129 (12.4) |
<0.001 |
| Prior CABG |
7 (0.6) |
25 (2.4) |
<0.001 |
| Situation at arrival |
| Heart failure |
141 (11.5) |
195 (18.5) |
<0.001 |
| Cardiogenic shock |
173 (14.1) |
179 (17.0) |
0.059 |
| Cardiopulmonary arrest |
100 (8.1) |
117 (11.1) |
0.017 |
| Referral from local clinic |
323 (26.3) |
165 (15.6) |
<0.001 |
| PCI at high-volume center (PCI ≥200/year)* |
1,102 (89.8) |
844 (79.9) |
<0.001 |
| Off-hour arrival** |
669 (55.0) |
676 (64.9) |
<0.001 |
| Procedure characteristics |
| Femoral approach |
1,052 (85.8) |
895 (84.8) |
0.51 |
| Radial approach |
172 (14.0) |
148 (14.0) |
0.99 |
| IABP |
211 (17.2) |
245 (23.2) |
<0.001 |
| VA-ECMO |
28 (2.3) |
35 (3.3) |
0.13 |
| LAD lesion |
593 (48.3) |
441 (41.8) |
0.002 |
| RCA lesion |
492 (40.1) |
427 (40.4) |
0.87 |
| LCX lesion |
99 (8.1) |
118 (11.2) |
0.012 |
| Type C lesion |
260 (21.5) |
249 (24.0) |
0.07 |
| Bifurcation lesion |
292 (24.3) |
261 (25.4) |
0.54 |
Data given as mean±SD or n (%). *Annual PCI volume ≥200; **arrival between 6 p.m. and 8 a.m on weekdays, or at any time on weekends or public holidays. BMI, body mass index; CABG, coronary artery bypass grafting; CAD, coronary arterial disease; CKD, chronic kidney disease; DTB, door-to-balloon; eGFR, estimated glomerular filtration rate; HD, hemodialysis; IABP, intra-aortic balloon pump; LAD, left anterior descending; LCX, left circumflex; MI, myocardial infarction; PCI, percutaneous coronary intervention; RCA, right coronary artery; VA-ECMO, veno-arterial extracorporeal membrane oxygenation.
The results of multivariable analysis are shown in
Figure 3. Presence of PAD, prior revascularization, arrival during off-hours, age >75 years, heart failure at arrival, and requirement for IABP or VA-ECMO were significant predictors of delay in DTB time, while PCI at high-volume centers, referral from local clinics, and LAD lesion were associated with shorter DTB time. In particular, PCI at high-volume centers was the strongest predictor of decreased DTB time delay (OR, 0.42; 95% CI: 0.32–0.55, P<0.001). An interaction did not exist between PCI volume and hour of presentation (for interaction, P=0.12).
DTB Time vs. Hospital Volume
The number of STEMI patients who underwent PCI ≤12 h after onset was 1,946 in high-volume centers and 337 in low-volume centers. Crude median DTB time in the high-volume centers was 86 min (IQR, 66–110 min) and 105.5 min (IQR, 77–135 min) in the low-volume centers. The crude mean proportion of achievement of DTB time ≤90 min in low-volume centers was 37.1% (n=125; range, 17.8–80.0%;
Figure S1).
Discussion
We analyzed DTB time in STEMI patients consecutively registered in a contemporary multicenter Japanese database, and found that, currently, half of the patients had DTB time >90 min. The predictors for DTB time delay was multifactorial, but there were significant variables suitable for intervention including PAD and off-hour arrival. Overall institutional volume was also associated with DTB time: high-volume institutions achieved shorter DTB times compared with low-volume institutions, and the trend was pronounced in recent years. It is important to determine the clinical characteristics and profiles of patients who undergo PCI in different regions, because such data are necessary to evaluate whether patients are being managed appropriately and in line with the available clinical guidelines and evidence-based medicine. This analysis supports the notion that regional (and individual) efforts are needed to improve DTB time, which is regarded globally as an important quality indicator of STEMI care.
Previous Studies and Implications for DTB Time in Japan
The present data imply that DTB time for Japanese STEMI patients is unsatisfactory in a considerable proportion of patients: 46.2% of the present patients received PCI after the recommended 90 min. More importantly, DTB time has remained unchanged during the study period (September 2008–December 2013), in contrast to that in Western countries.19
Internationally, DTB time has been a major focus in quality assessment for primary PCI for the past decade,9
and Western DTB time has been found to decrease in recent years. For example, the national registry of PCI in the US (NCDR) showed that the median DTB time was 86 min (IQR, 65–109 min) in 2005, but was shortened to 63 min (IQR, 47–80 min) by 2011.4
In contrast, the median DTB time in a multicenter registry conducted between January 2005 and December 2007 in Japan (CREDO-Kyoto) was 90 min (IQR, 60–132 min).15
The present study has noted similar results in the more contemporary era of PCI, and highlights the need for progress in this area. Another study from a Japanese multicenter registry (J-AMI registry) noted a better result than the present one, in that median DTB time was 42 min (IQR, 28–66 min) for May–October 2011.21
Those participants, however, were enrolled from only registered institutions of the Japanese Association of Cardiovascular Intervention and Therapeutics and not from all institutions, hence that registry has a potential selection bias, and therefore those findings must be interpreted with caution.
Since 2008, the Japanese Circulation Society guidelines for STEMI management have incorporated a DTB time recommendation.22
The recommendation has been further emphasized in more recent guidelines: when the guideline was revised in 2013, DTB time <90 min was recommended (class I) in all STEMI patients presenting ≤12 h of symptom onset. Moreover, in April 2014, the reimbursement rules for primary PCI were altered. When DTB time ≤90 min is not achieved, the reimbursement rate for each procedure is cut by 29%.23
Such pay for performance (P4P) initiatives (to a smaller extent) have improved the quality of care for STEMI patients in the USA,24,25
but its effect on the actual clinical outcome remains controversial. Further studies are needed to assess the implication of P4P in DTB time in Japan.
Clinical Predictors of Delay in DTB Time
Most of the baseline characteristics of the present STEMI patients were similar to previously published data, although the Japanese patients were generally older and had a lower burden of predisposing cardiac risk factors or comorbidities: a smaller percentage of patients had PAD or previous revascularization procedures.16
Despite these differences, predictors of prolonged DTB time were not substantially different from those in Western countries.11–13,26
Comorbid conditions would lead to complexity of the infarct or non-infarct related artery. In addition, difficulties in obtaining vascular access in these patients, particularly in those with PAD, or additional time required to stabilize respiratory status and/or hemodynamic derangement may all lead to prolonged DTB time. The latter is reflected in the proportion of patients with congestive heart failure or those requiring mechanical device support (e.g., VA-ECMO or IABP).27
These conditions are not currently indications for intervention, and it is likely that these will continue to predispose to prolonged DTB times, given the aging population in Japan, but caregivers should at least be made aware that these conditions would likely delay reperfusion. Further, rigorous adjustment or even separate classification of these high-risk patients may be necessary to justify DTB time assessment as a quality indicator.
In contrast, specific interventions to decrease DTB time should be targeted. For example, the time interval between activation of the cardiac on-call team and commencement of the procedure accounts for a substantial proportion of the delay in primary PCI for STEMI patients. In the present analysis, this was reflected in the longer DTB time during night-time and weekend presentation. This may be improved by increasing the efficiency of on-call cardiac catheterization.28
We also found that high-volume centers were more likely to achieve shorter DTB times compared with low-volume centers. The reason for this is not entirely clear, but previous studies in both medical and surgical settings have demonstrated that a lower patient load can impair efficiency in patient care.29,30
Traditionally, Japan has a higher number of PCI-capable hospitals compared with Western countries due to the coverage of social health insurance.17
Transportation of patients to primary PCI centers by emergency medical service is free and highly accessible,31
but, as a trade-off, primary PCI volume has diverged, and the number of primary PCI performed in each hospital is relatively small. Importantly, several studies have linked higher hospital PCI volume and greater adherence to evidence-based medicine to better outcomes.32,33
This inverse association between primary PCI volume and in-hospital mortality has been reported for other Japanese cohorts.34
The present results indicate that the balancing of the number of PCI-capable facilities and maintenance of performance indicators such as DTB time may be challenging. Further studies to delineate these relationships could facilitate the international standardization of health-care delivery.35
DTB Time and In-Hospital Mortality: Current Status
Improving both in-hospital and post-discharge care remain key targets for enhancing long-term outcomes after STEMI. Recent studies have suggested increased risk in patients undergoing primary PCI owing to increased complexity of comorbidities presenting with acute MI.9
Consistent with these studies, the present data suggest a correlation between aging patients and multiple comorbidities with prolonged DTB time. These patients are typically more likely to have delayed hospital arrival time,36
and are less likely to be treated with evidence-based medical therapy (e.g., β-blockers, angiotensin-converting enzyme inhibitors or angiotensin II receptor blockers, and statins).37
Still, Nallamothu et al showed that shorter patient-specific DTB time was strongly and consistently associated with lower risk-adjusted in-hospital and 6-month mortality.4
Importantly, the present study showed that DTB time tends to be prolonged in patients with comorbidities such as CKD or concomitant vascular disease (e.g., PAD or previous revascularization). Debate persists as to whether the shortening of DTB time in high-risk patients improves outcome.19,24
A solution may involve the detailed consideration of medical resource allocation, system improvement, and disease management, but this warrants further discussion.
Study Limitations
There were several limitations in the present study. First, the study had the inherent limitations of any non-randomized observational research: it is possible that unmeasured confounders could have contributed to prolonged DTB time, even after rigorous measurement and recording of key clinical variables. As quoted, the present registry was developed in accordance with NCDR version 4.1, and did not record non-quantifiable parameters (e.g., presence of dementia or physical frailty) or out-of-hospital variables such as arrival time at the initial satellite clinic, method of transportation to the initial hospital, use of prehospital 12-lead electrocardiography, or treatment within emergency medical systems. Specifically, the use of IABP included patients who required IABP during the procedure. We could not define whether IABP was used before or after first device use for the culprit artery. Moreover, we did not record key clinical variables that might have contributed to differences between high- and low-volume centers. For instance, parameters surrounding the emergency department (ED) or catheterization laboratory, especially door-to-electrocardiogram time, patient load in ED (i.e., average number of patients treated by each physician), the number of interventional cardiologists or other medical staff members who were on call, the interval between time of page and arrival of staff at the catheterization laboratory, or whether timely data feedback and analysis were provided to members of the STEMI care team. A multivariable-adjusted logistic regression model was used to investigate differences in high- and low-volume centers in the present dataset (Figure S2). Subgroup analysis in high-volume centers demonstrated a similar tendency with the overall model. In low-volume centers, there was no predictive value for DTB time delay due to PAD, prior revascularizations, age >75 years, heart failure at arrival, use of IABP/VA-ECMO, or LAD lesion. This study may be statistically underpowered because of the small population size, but patients who arrived at low-volume centers in off-hours were more likely to have prolonged DTB time (OR, 2.22; 95% CI: 1.32–3.74; P=0.003).
Figure S3
shows the annual trends of median DTB time in the high- and low-volume centers. In 2010, the median DTB time was 88 min (IQR, 69–108 min) in the high-volume centers and 90 min (IQR, 60–117 min) in the low-volume centers (P=0.78). It seems that the median DTB time worsened in the low-volume centers after 2011, which may be due to the inclusion of different hospitals each year (e.g., the number of participating hospitals and the mean percentage of achievement of DTB time <90 min in the low-volume centers differed with year). Second, onset time of the event was collected in only a limited number of patients (2012–2013). Despite this limitation, we assessed the total ischemic time in 13.4% of the patients (n=305). Overall median symptom onset-to-balloon time was 235 min (IQR, 153.5–357.5 min). There was no difference in onset-to-balloon time between high- (228 min: IQR, 165–325 min) and low-volume centers (236 min: IQR, 153–364 min). Hence, it is unlikely that difference in DTB times is attributed to time interval differences in the field. Rather, the difference in DTB time with institution volume seemed to have been due to institutional factors (e.g., management within the hospital). Third, the present numbers are relatively small, particularly for the analysis of in-hospital mortality, therefore the clinical outcomes must be interpreted with caution. It is still unknown whether increasing the percentage of patients with DTB time ≤90 min would actually contribute significantly to improve STEMI outcome. Fourth, several key variables (e.g., ejection fraction or maximum creatinine kinase after primary PCI) that are considered predictors of in-hospital death were not measured in the current registry. Last, the present cases of suspected STEMI were based on cardiologist review. Other studies have used different criteria such as emergency physician decision without cardiologist review, which may result in a higher STEMI rate.
Conclusions
In the present prospective regional dataset maintained by trained personnel, almost half of the STEMI patients did not achieve the target DTB time. Focus on the elderly and on multiple comorbidities, and on modifiable factors such as off-hour performance of PCI, may aid in its improvement. Further efforts are also needed to improve patient care in Japan, with particular emphasis on medical resource allocation, system improvement, and disease management.
Acknowledgments
We are indebted to all study coordinators, investigators, and patients who participated in the JCD-KiCS registry. This research was supported by a grant from the Ministry of Education, Culture, Sports, Science, and Technology, Japan (KAKENHI No. 16H05215, 25460630 and 25460777) and by Grants-in-Aid for Scientific Research from the Japan Society for the Promotion of Science.
Disclosures
S.K. received an unrestricted research grant for Department of Cardiology, Keio University School of Medicine from Bayer Pharmaceutical and Pfizer Japan. The other authors declare no conflict of interest.
Appendix I
Site Investigators
Yohei Numasawa, Toshiki Kuno, Hiroyuki Motoda, Masaki Kodaira, Ryota Tabei (Ashikaga Red Cross Hospital);
Soushin Inoue, Iwao Nakamura, Tomohiro Matsuhashi (Hino Municipal Hospital);
Takashi Matsubara, Shunsuke Takagi, Taku Inohara (Hiratsuka City Hospital and Isehara Kyodo Hospital);
Koichiro Sueyoshi, Keishu Li, Masashi Takahashi (Kawasaki City Municipal Hospital);
Yutaka Okada
(Eiju General Hospital);
Yuichiro Maekawa, Shunsuke Yuasa, Hideaki Kanazawa, Kentaro Hayashida, Takashi Kawakami, Fumiaki Yashima, Mai Kimura, Keitaro Akita (Keio University School of Medicine);
Masahiro Suzuki, Takaharu Katayama, Keisuke Matsumura, Tomohiko Ono, Hanako Tokuda (National Hospital Organization Saitama National Hospital);
Yukihiko Momiyama, Munehisa Sakamoto, Jun Fuse, Kojiro Tanimoto, Yukinori Ikegami, Kohei Inagawa (National Hospital Organization Tokyo Medical Center);
Susumu Nakagawa, Toshiyuki Takahashi, Taku Hasegawa, Ayaka Endo, Makoto Taeki (Saiseikai Central Hospital);
Shigetaka Noma, Takashi Yagi, Kenichiro Shimoji, Koji Ueno, Satoshi Mogi (Saiseikai Utsunomiya Hospital);
Takashi Koyama, Shiro Ishikawa, Hideaki Kanki, Takashi Akima, Masahito Munakata (Saitama City Hospital);
Atsushi Mizuno
(St Luke’s International Hospital);
Hideo Mitamura, Masaru Shibata, Kazunori Moritani, Daisuke Shinmura, Toshimi Kageyama (Tachikawa Hospital);
Takahiro Oki, Yoshinori Mano, Hiroaki Sukegawa (Tokyo Dental College Ichikawa General Hospital);
Kouji Negishi, Takahiro Koura, Hiroyuki Yamakawa (Yokohama Municipal Citizen’s Hospital).
Clinical Coordinators
Junko Susa, Ayano Amano, Hiroaki Nagayama, Miho Umemura, Itsuka Saito and Ikuko Ueda.
Supplementary Files
Supplementary File 1
Figure S1.
Rate of door-to-balloon time ≤90 min vs. hospital.
Figure S2.
Multivariable predictors of door-to-balloon (DTB) time delay in high- and low-volume centers.
Figure S3.
Median door-to-balloon time vs. hospital percutaneous coronary intervention (PCI) volume and year.
Please find supplementary file(s);
http://dx.doi.org/10.1253/circj.CJ-16-0905
References
- 1.
Bonnefoy E, Lapostolle F, Leizorovicz A, Steg G, McFadden EP, Dubien PY, et al. Primary angioplasty versus prehospital fibrinolysis in acute myocardial infarction: A randomised study. Lancet 2002; 360: 825–829.
- 2.
Eagle KA, Nallamothu BK, Mehta RH, Granger CB, Steg PG, Van de Werf F, et al. Trends in acute reperfusion therapy for ST-segment elevation myocardial infarction from 1999 to 2006: We are getting better but we have got a long way to go. Eur Heart J 2008; 29: 609–617.
- 3.
Gibson CM, Pride YB, Frederick PD, Pollack CV Jr, Canto JG, Tiefenbrunn AJ, et al. Trends in reperfusion strategies, door-to-needle and door-to-balloon times, and in-hospital mortality among patients with ST-segment elevation myocardial infarction enrolled in the National Registry of Myocardial Infarction from 1990 to 2006. Am Heart J 2008; 156: 1035–1044.
- 4.
Nallamothu BK, Normand SLT, Wang Y, Hofer TP, Brush JE, Messenger JC, et al. Relation between door-to-balloon times and mortality after primary percutaneous coronary intervention over time: A retrospective study. Lancet 2015; 385: 1114–1122.
- 5.
Rathore SS, Curtis JP, Chen J, Wang Y, Nallamothu BK, Epstein AJ, et al. Association of door-to-balloon time and mortality in patients admitted to hospital with ST elevation myocardial infarction: National cohort study. BMJ 2009; 338: b1807.
- 6.
Japanese Circulation Society. 2013 Guidelines for the management of patients with ST-elevation acute myocardial infarction. http://www.j-circ.or.jp/guideline/pdf/JCS2013_kimura_h.pdf (in Japanese) (accessed November 16, 2011).
- 7.
American College of Emergency Physicians; Society for Cardiovascular Angiography and Interventions, O’Gara PT, Kushner FG, Ascheim DD, Casey DE Jr, Chung MK, de Lemos JA, et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 2013; 61: e78–e140.
- 8.
Jacobs AK, Antman EM, Ellrodt G, Faxon DP, Gregory T, Mensah GA, et al. Recommendation to develop strategies to increase the number of ST-segment-elevation myocardial infarction patients with timely access to primary percutaneous coronary intervention. Circulation 2006; 113: 2152–2163.
- 9.
Krumholz HM, Bradley EH, Nallamothu BK, Ting HH, Batchelor WB, Kline-Rogers E, et al. A campaign to improve the timeliness of primary percutaneous coronary intervention: Door-to-Bballoon JACC Cardiovasc Interv 2008; 1: 97–104.
- 10.
Angeja BG, Gibson CM, Chin R, Frederick PD, Every NR, Ross AM, et al. Predictors of door-to-balloon delay in primary angioplasty. Am J Cardiol 2002; 89: 1156–1161.
- 11.
Blankenship JC, Skelding KA, Scott TD, Berger PB, Parise H, Brodie BR, et al. Predictors of reperfusion delay in patients with acute myocardial infarction undergoing primary percutaneous coronary intervention from the HORIZONS-AMI trial. Am J Cardiol 2010; 106: 1527–1533.
- 12.
Parikh SV, Jacobi JA, Chu E, Addo TA, Warner JJ, Delaney KA, et al. Treatment delay in patients undergoing primary percutaneous coronary intervention for ST-elevation myocardial infarction: A key process analysis of patient and program factors. Am Heart J 2008; 155: 290–297.
- 13.
Swaminathan RV, Wang TY, Kaltenbach LA, Kim LK, Minutello RM, Bergman G, et al. Nonsystem reasons for delay in door-to-balloon time and associated in-hospital mortality: A report from the National Cardiovascular Data Registry. J Am Coll Cardiol 2013; 61: 1688–1695.
- 14.
Terkelsen CJ, Sørensen JT, Maeng M, Jensen LO, Tilsted HH, Trautner S, et al. System delay and mortality among patients with STEMI treated with primary percutaneous coronary intervention. JAMA 2010; 304: 763–771.
- 15.
Shiomi H, Nakagawa Y, Morimoto T, Furukawa Y, Nakano A, Shirai S, et al. Association of onset to balloon and door to balloon time with long term clinical outcome in patients with ST elevation acute myocardial infarction having primary percutaneous coronary intervention: Observational study. BMJ 2012; 344: e3257.
- 16.
Kohsaka S, Miyata H, Ueda I, Masoudi FA, Peterson ED, Maekawa Y, et al. An international comparison of patients undergoing percutaneous coronary intervention: A collaborative study of the National Cardiovascular Data Registry (NCDR) and Japan Cardiovascular Database-Keio interhospital Cardiovascular Studies (JCD-KiCS). Am Heart J 2015; 170: 1077–1085.
- 17.
Ui S, Chino M, Isshiki T. Rates of primary percutaneous coronary intervention worldwide. Circ J 2005; 69: 95–100.
- 18.
Ikegami N, Yoo BK, Hashimoto H, Matsumoto M, Ogata H, Babazono A, et al. Japanese universal health coverage: Evolution, achievements, and challenges. Lancet 2011; 378: 1106–1115.
- 19.
Menees DS, Peterson ED, Wang Y, Curtis JP, Messenger JC, Rumsfeld JS, et al. Door-to-balloon time and mortality among patients undergoing primary PCI. N Engl J Med 2013; 369: 901–909.
- 20.
Japanese Association of Cardiovascular Intervention and Therapeutics. Condition of educational institution. http://www.cvit.jp/facilities/training/ (accessed November 16, 2011).
- 21.
Nakamura M, Yamagishi M, Ueno T, Hara K, Ishiwata S, Itoh T, et al. Current treatment of ST elevation acute myocardial infarction in Japan: Door-to-balloon time and total ischemic time from the J-AMI registry. Cardiovasc Interv Ther 2013; 28: 30–36.
- 22.
Japanese Circulation Society. 2008 Guidelines for the management of patients with ST-elevation myocardial infarction. http://www.j-circ.or.jp/guideline/pdf/JCS2008_takano_h.pdf (in Japanese) (accessed November 16, 2011).
- 23.
Japanese Ministry of Health, Labour and Welfare. Revision in medical treatment fee. http://www.mhlw.go.jp/stf/seisakunitsuite/bunya/0000032996.html (in Japanese) (accessed November 16, 2011).
- 24.
Flynn A, Moscucci M, Share D, Smith D, LaLonde T, Changezi H, et al. Trends in door-to-balloon time and mortality in patients with ST-elevation myocardial infarction undergoing primary percutaneous coronary intervention. Arch Intern Med 2010; 170: 1842–1849.
- 25.
Bucholz EM, Butala NM, Normand SL, Wang Y, Krumholz HM. Association of guideline-based admission treatments and life expectancy after myocardial infarction in elderly Medicare beneficiaries. J Am Coll Cardiol 2016; 67: 2378–2391.
- 26.
Gruberg L, Hellkamp AS, Thomas LE, de Lemos JA, Scirica BM, Hilliard A, et al. The association of previous revascularization with in-hospital outcomes in acute myocardial infarction patients: Results from the National Cardiovascular Data Registry. JACC Cardiovasc Interv 2015; 8: 1954–1962.
- 27.
Wu AH, Parsons L, Every NR, Bates ER; Second National Registry of Myocardial Infarction. Hospital outcomes in patients presenting with congestive heart failure complicating acute myocardial infarction: A report from the Second National Registry of Myocardial Infarction (NRMI-2). J Am Coll Cardiol 2002; 40: 1389–1394.
- 28.
Sorita A, Ahmed A, Starr SR, Thompson KM, Reed DA, Prokop L, et al. Off-hour presentation and outcomes in patients with acute myocardial infarction: Systematic review and meta-analysis. BMJ 2014; 348: f7393.
- 29.
Kontos MC, Wang Y, Chaudhry SI, Vetrovec GW, Curtis J, Messenger J, et al. Lower hospital volume is associated with higher in-hospital mortality in patients undergoing primary percutaneous coronary intervention for ST-segment-elevation myocardial infarction: A report from the NCDR. Circ Cardiovasc Qual Outcomes 2013; 6: 659–667.
- 30.
Horwitz LI, Lin Z, Herrin J, Bernheim S, Drye EE, Krumholz HM, et al. Association of hospital volume with readmission rates: A retrospective cross-sectional study. BMJ 2015; 350: h447.
- 31.
Japanese Association of Cardiovascular Intervention and Therapeutics. List of educational institutions. http://www.cvit.jp/files/list_doctor-facility/facility/by_pref-number.pdf (in Japanese) (accessed November 16, 2016).
- 32.
Kumbhani DJ, Cannon CP, Fonarow GC, Liang L, Askari AT, Peacock WF, et al. Association of hospital primary angioplasty volume in ST-segment elevation myocardial infarction with quality and outcomes. JAMA 2009; 302: 2207–2213.
- 33.
Canto JG, Every NR, Magid DJ, Rogers WJ, Malmgren JA, Frederick PD, et al. The volume of primary angioplasty procedures and survival after acute myocardial infarction: National Registry of Myocardial Infarction 2 Investigators. N Engl J Med 2000; 342: 1573–1580.
- 34.
Kuwabara H, Fushimi K, Matsuda S. Relationship between hospital volume and outcomes following primary percutaneous coronary intervention in patients with acute myocardial infarction. Circ J 2011; 75: 1107–1112.
- 35.
Pottenger BC, Diercks DB, Bhatt DL. Regionalization of care for ST-segment elevation myocardial infarction: Is it too soon? Ann Emerg Med 2008; 52: 677–685.
- 36.
Goldberg RJ, Spencer FA, Fox KA, Brieger D, Steg PG, Gurfinkel E, et al. Prehospital delay in patients with acute coronary syndromes (from the Global Registry of Acute Coronary Events [GRACE]). Am J Cardiol 2009; 103: 598–603.
- 37.
Lee JH, Yang DH, Park HS, Cho Y, Jeong MH, Kim YJ, et al. Suboptimal use of evidence-based medical therapy in patients with acute myocardial infarction from the Korea Acute Myocardial Infarction Registry: Prescription rate, predictors, and prognostic value. Am Heart J 2010; 159: 1012–1019.