Article ID: CJ-16-0980
Article ID: CJ-16-0980
Vascular risk factors such as hypertension, obesity and diabetes have been focused on as potentially modifiable risk factors for Alzheimer disease, as well as vascular dementia,1 because dementia is considered to be induced via disruption of neurovascular coupling, with vascular disorder as one possible mechanism.2 One vascular risk factor, mid-life high blood pressure (BP), is associated with poor cognitive performance, compared with late-life high BP.3 Launer et al demonstrated in the Honolulu Heart Program/Honolulu Asia Aging Study the possibility that lowering mid-life systolic BP using antihypertensive drugs may reduce late-life dementia.4 Therefore, antihypertensive drugs are expected to be effective as antidementia drugs (Figure). Among the antihypertensive drugs, calcium-channel blockers (CCBs) and renin-angiotensin system (RAS) blockers, such as angiotensin-converting enzyme inhibitors (ACEIs) and angiotensin type 1 receptor blockers (ARBs), showed benefit in preventing cognitive decline in several randomized, double-blind placebo-controlled trials. For example, in the SYSTolic hypertension in EURope (SYST-EUR) trial, treatment with a CCB, nitrendipine, demonstrated prevention of dementia,5 and in the Perindopril pROtection aGainst REcurrent Stroke (PROGRESS) study, an ACEI, perindopril,6 showed a preventive effect on cognitive decline.
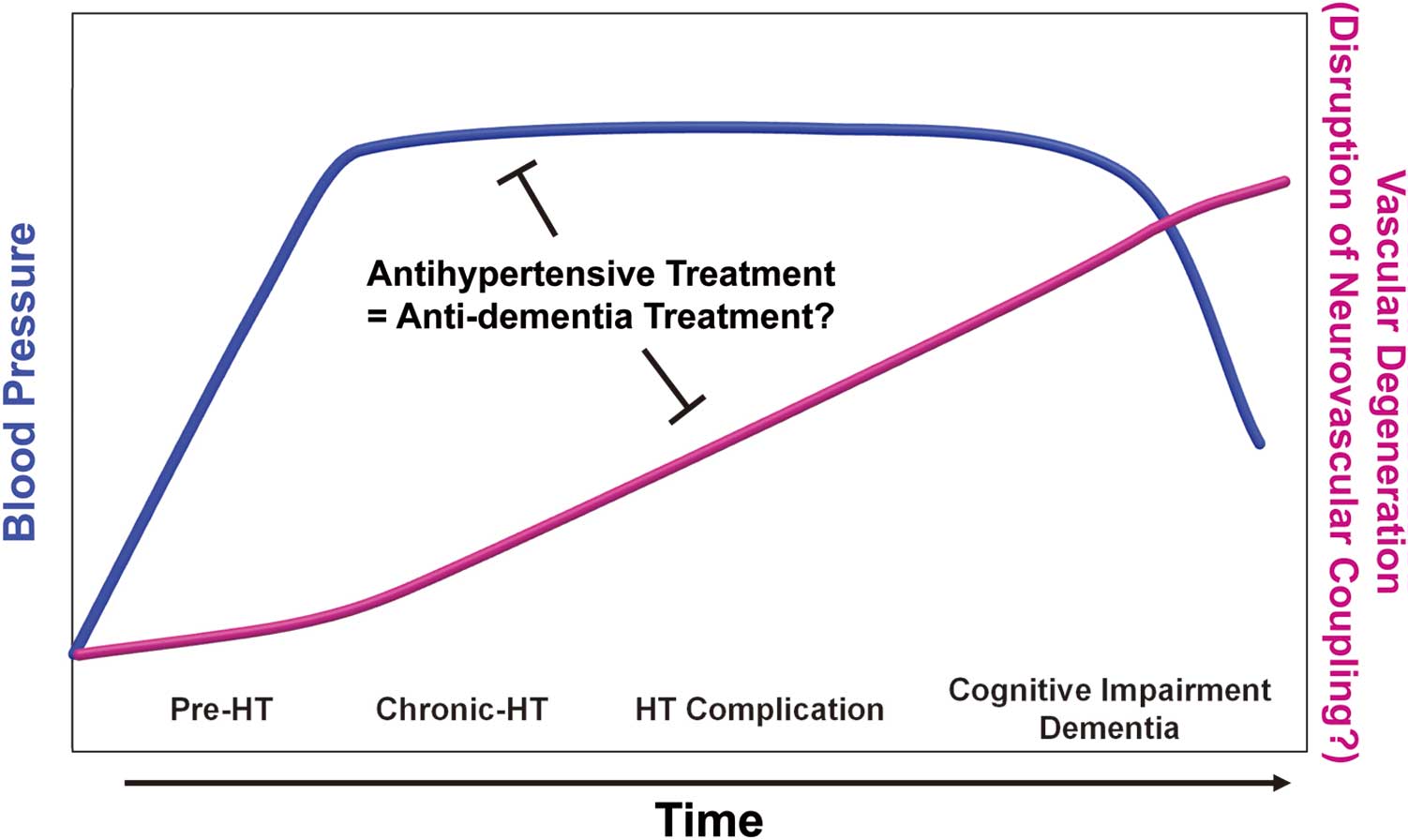
Effect of antihypertensive drugs on dementia and possible relationship between hypertension (HT) and vascular degeneration.
Article p ????
In this issue of the Journal, Hwang et al report their large population-based cohort study using the database of the Korean National Health Insurance Service to focus on dementia, and they show that CCB users had a significantly reduced risk of dementia (adjusted hazard ratio for total dementia 0.81, for Alzheimer disease 0.80, and for vascular dementia 0.81).7 Overall, the risk reduction ratio was around 20% in CCB users. In a basic experiment, Kishi and Sunagawa demonstrated that combination therapy with atorvastatin and a CCB, amlodipine, inhibited sympathetic nervous system activation and improved cognitive function in hypertensive rats via an antioxidant effect in the rostral ventrolateral medulla, independent of the BP-lowering effect.8 Tsukuda et al also reported a preventive effect of a non-hypotensive dose of nifedipine on cognitive decline in diabetic mice, with a decrease in superoxide anion production in the brain and an increase in cerebral blood flow.9 Moreover, CCBs such as amlodipine are reported to have vascular protective effects via an increase in endothelial nitric oxide.10 Katusic and Austin clearly showed a neurovascular protective function of endothelial nitric oxide.11 Therefore, a CCB-induced vascular protective effect is one of the possible mechanisms of preventing the incidence of dementia (Figure).
However, this study has limitations. The first is a methodological problem. Previously, Hsu et al demonstrated that ARB treatment was not significantly associated with a reduction of risk of Alzheimer disease in Asian patients with essential hypertension, using a population-based cohort database in Taiwan.12 In a commentary, Katayama and Hasebe pointed out that a study limitation was the study not being a prospective double-blind placebo-controlled study.13 A similar criticism can be raised about the present study. The second problem is the characteristics of the CCB users. CCBs are widely used with other antihypertensive drugs, and many hypertensive subjects are treated with a combination of RAS blocker and CCB. Therefore, comparison of patients on CCB monotherapy and on monotherapy with other hypertensive drugs such as RAS blockers is needed. More detailed analysis is necessary to determine the direct effect of CCBs on dementia.
On the other hand, Peters et al reported a systematic review of CCB use and cognitive decline/dementia in the elderly.14 They concluded that there is no clear evidence to suggest an increased or decreased risk of cognitive decline or dementia in elderly CCB users, because of the lack of a robust clinical trial with many hypertensive subjects with a long follow-up to resolve this issue. The present study shows evidence for a preventive effect of CCBs on dementia; however, to elucidate their actual effect on dementia will be a challenge.
None.