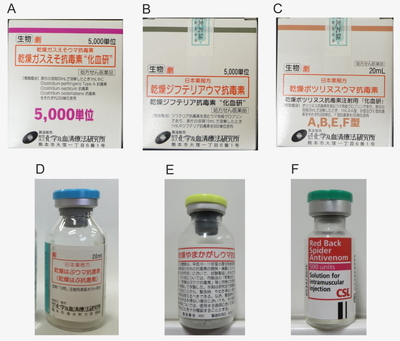
Specific Serum Therapies
Gas gangrene
Currently, clostridial gas gangrene, a life-threatening muscle infection, is rarely
reported,16 in contrast to the
relatively frequently encountered non-clostridial gas gangrene. This fact has been
attributed to the aging of society.17,18 The
main etiologic agent in the former condition, α-toxin secreted by Clostridium
perfringens, causes intravascular hemolysis followed by severe anemia,
disseminated intravascular coagulopathy (DIC),19,20 and
multiple organ failure (Table 2).
Table 2
Basic information about toxins and venoms
|
Toxin/venom |
Typical symptoms |
| Gas gangrene |
α-Toxin |
Hemolysis and disseminated intravascular
coagulation |
| Diphtheria |
Diphtheria toxin |
Myocarditis and local neuropathies (paralysis of the
soft palate and posterior pharyngeal wall), followed by cranial neuropathies
(usually oculomotor and ciliary, followed by facial or laryngeal paralyses) |
| Botulism |
Clostridium botulinum toxin
(A,B,C,D,E,F,G,H,I) |
Cranial neuropathies associated with symmetric
descending
weakness |
| Tetanus |
Tetanus toxin |
Opisthotonos, dysphagia, excessive sweating, and
fever |
| Mamushi (Gloydius blomhoffii) |
Mamushi venom |
Local pain and swelling |
| Habu (Protobothrops
flavoviridis) |
Habu venom |
Severe local swelling, necrosis, and bleeding at the
bite site |
| Yamakagashi (Rhabdophis
tigrinus) |
Prothrombin activator |
Disseminated intravascular coagulation with a
fibrinolytic
phenotype |
| Redback spider (Latrodectus
hasselti) |
α-Latrotoxin |
Severe pain, sweating, nausea, and abdominal
pain |
Gas gangrene antitoxin comprises equine serum immunoglobulins raised against three
specific gas gangrene toxins (C. perfringens type A, C.
septicum, and C. oedematiens), and has been approved for
commercial distribution.6 However, this
product is no longer available in the United States because of poor efficacy and severe
allergic reactions.21
Despite the decrease in reported cases of clostridial gas gangrene, the incidence of
C. perfringens septicemia without gas gangrene has been increasing. Van
Bunderen et al. retrospectively reviewed cases of C. perfringens
septicemia that rapidly progressed to intravascular hemolysis, metabolic acidosis, and
death within a few hours after patient admission.22 In their review, the mortality rate was >80% despite treatment
with high-dose antibiotics and surgical debridement. Therefore, we must redefine
conventional standard treatments by re-examining the pathophysiology of
Clostridium infections. To this end, we recommend that administration
of antitoxin along with antibiotics should be considered as early as possible to
neutralize the toxin.21
Diphtheria
Diphtheria is associated with an infection of the gram-positive bacillus
Corynebacterium diphtheriae. Specifically, diphtheria toxin acts
intracellularly to cause cell death, particularly in the diaphragm and myocardium.
Corynebacterium diphtheriae infection may lead to respiratory disease,
cutaneous disease, or an asymptomatic carrier state (Table 2). In developed countries, the estimated mortality associated with
diphtheria range from 5% to 10%.23
Corynebacterium ulcerans, which shares a similar, but not identical,
toxin antigen, induces a rare diphtheria-like infection, and isolated cases of this
illness have been identified not only in the United States24 but also in Japan, where a related fatality was
reported23,24. Similar to Corynebacterium
diphtheria, Corynebacterium ulcerans can produce diphtheria
toxin, leading to a life-threatening disease that requires urgent treatment with
diphtheria antitoxin and macrolide antibiotics.25,26
Botulism
Botulism, a potentially life-threatening neuro-paralytic syndrome caused by a neurotoxin
produced by C. botulinum, is generally characterized by the acute onset
of bilateral cranial neuropathies and symmetrical descending weakness. Botulism cases can
be classified as foodborne, infant, wound, adult enteric infectious, inhalational, and
iatrogenic, based on the mode of acquisition.27 Notably, infant and adult enteric infectious botulisms occur in Japan
at a rate of approximately one case per year. The currently available heptavalent botulism
antitoxin is administered only to adults because its efficacy and safety have not been
determined for infants28,29; to
date, all efficacy studies have been conducted in animals because it is not feasible or
ethical to conduct such studies in human populations. In an attempt to evaluate human
efficacy, Tacket et al. retrospectively evaluated data of 132 patients with type A
foodborne botulism and found that patients treated with antitoxin had decreased mortality
rates compared with untreated patients.29 However, details such as the severity of foodborne botulism and
comorbidities were not compared.
In Japan, antitoxins to the A, B, E, and F botulism toxins are manufactured, stored in a
national stockpile, and provided for the treatment of primary severe adult dietary food
poisoning. However, with regard to the manufacturing of botulinum equine antitoxin
preparations worldwide, the ranch maintenance required for equine management and securing
the human resources for manufacturing plants remain as obstacles in many countries.
Additional difficulties associated with the market economy and technology inheritance have
led to the cessation of antitoxin production in many countries. Accordingly, antitoxin
stockpiles held by countries, such as Japan, have been used during outbreaks for the
humanitarian rescue of many patients in countries that do not stockpile
antitoxins30,31. In addition, the potential nature of
botulinum toxin as a weapon of terrorism has led to the need for national antitoxin
stockpiles as a counter-terrorism measure.31
Tetanus
Tetanus is caused by a toxin produced by C. tetani, which is found in
soil, human feces, and objects lying on the ground. This tetanus toxin blocks
neurotransmission by cleaving membrane proteins, leading to muscle spasms of the jaw,
chest, neck, back, abdominal muscles, buttocks, and back muscles, a condition referred to
as opisthotonos. Other symptoms of tetanus include drooling, excessive sweating, fever,
hand or foot spasms, irritability, dysphagia, and urinary or rectal incontinence (Table 2). The annual incidence of tetanus in Japan
has remained consistent at approximately100 cases, with a 10% mortality rate.32 Tetanus immunoglobulin (TIG) is derived from
human serum and has been approved for commercial distribution. TIG neutralizes only the
unbound endotoxin produced by C. tetani; this agent possesses neither
antibacterial activity nor the capacity to prevent bacterial growth, and cannot restore
organ function.33 The tetanus toxin
initially binds to peripheral nerve terminals to cause the clinical symptoms.2,34. Therefore, theoretically, TIG does not resolve clinical
symptoms, although such assertions are likely to be incorrect. However, Vollman et al.
reported an interesting case of tetanus in which the patient’s symptoms were resolved
after human TIG administration. Thirteen hours after TIG administration, the patient had
an increased range-of-motion in the lower jaw and decreased neck pain. Approximately 27 h
after TIG administration, the patient recovered the full range-of-motion in his neck and
was able to move his jaw more completely. We note that no additional pharmacologic
treatment was given in that case.2,35
Under the Preventive Vaccination Law, enacted in Japan in 1968, four doses of diphtheria,
tetanus, and pertussis vaccine are administered during infancy, and a vaccine against
diphtheria and tetanus is administered at the age of 11–12 years.36,37 However, the immunity induced by vaccination wanes after
approximately 10 years.38 In 2008,
Takahashi et al. reported that individuals older than 45 years exhibited only 10% of the
protective level of antibody titer for tetanus39; in other words, tetanus preventive measures are insufficient. In
contrast, in the United States, the reported level of seroprotection against tetanus in
adults older than 65 years is approximately 80%.40 In Japan, adult antibody titers remain remarkably low when compared
to those in other regions, and twice as many tetanus patients are reported in Japan than
in the United States, with an accompanying high mortality rate (approximately
10%).39 Physicians should bear in
mind that proper passive immunization with TIG for tetanus should be considered in
patients older than 50 years, given the existing low immunity levels.
Mamushi (Gloydius blomhoffii) bites
Mamushi is a pit viper with fangs about 5 mm long with very thin tips (Fig. 2A).

Approximately 2000–3000 mamushi bites occur annually in Japan, and mamushi venom is
generally associated with local pain and swelling (Table 2). However, no previous randomized controlled trials (RCTs) or
meta-analyses have examined the effects of antivenom. Hifumi et al. conducted a large,
multi-center, population-based study41
of 234 mamushi bite cases and found that among severe cases (redness and swelling beyond
the elbow or knee joint), patients who received mamushi antivenom had significantly
shorter hospital stays compared to those who were administered cepharanthine
(P = 0.03). In contrast, no significant difference in the duration of
hospital stay was observed between the two groups for mild cases (redness and swelling
limited to the wrist or foot) (P = 0.77). In other words, mamushi
antivenom effectively reduces the hospital stay for patients with severe mamushi
bites.41 Until 1990, antivenom was
usually administered subcutaneously or intramuscularly to avoid adverse reactions, which
were of great concern. Theoretically, intravenous administration of antivenom leads to
earlier venom neutralization compared with subcutaneous or intramuscular administration.
We recommend antivenom administration in patients with a grade >III mamushi bite, based
on our previously reported data.13,41 Other
types of snake antivenom, such as yamakagashi or habu antivenom, cannot neutralize mamushi
venom.
Habu (Protobothrops flavoviridis) bites
Habu is the most dangerous of the three snakes considered here because it is large,
reaching up to 2 m in length, and is the most aggressive. Habu fangs are tubular and
1.5–2 cm in length (Fig. 2B). Habu venom causes
extremely severe local swelling, necrosis, and bleeding at the bite site13 (Table
2). To date, five types of pit vipers are known to inhabit Okinawa and Amami
islands, and habu bites are limited to areas outside of the Japanese main island. However,
the shifts promoted by climate change and increasingly intensive interactions between
people have led to concerns regarding the potential for increased frequencies of habu
bites on the main island.42
Although habu antivenom is considered effective when administered after a bite, no RCTs
or meta-analyses have examined the effects of this antivenom. Okinawa prefecture is known
to house a large population of habu, and, accordingly, it has a higher rate of habu
antivenom use compared with that of the Amami islands. No deaths from habu bites have been
reported in the past 12 years in Okinawa (2004–2015, no deaths in 603 cases).43 However, between 1965 and 1969,
approximately 24 deaths were reported among 1770 cases in Okinawa because of the
unavailability of habu antivenom.43
Recently, Nishimura et al. reported 86 cases of habu bites from 2003 to 2014 in Amami
Ohshima, a known habu habitat in Kagoshima prefecture.44 Good clinical outcomes were reported in this area, with 97.7% (84/86
patients) receiving antivenom therapy and a mortality rate of only 1.1% (1/86 cases). In
contrast, the mortality rate reported in the same area in 1978 was 10%.45 In summary, habu antivenom therapy appears
to decrease mortality and should be considered when treating habu bites.46,47
Yamakagashi (Rhabdophis tigrinus) bites
Yamakagashi grow to about 1 m in the plains and 1.5 m in the hills and mountains of Japan
(excluding Hokkaido). The fangs of yamakagashi are not tubular, and the venom gland duct
opens at the base of the fang (Fig. 2C).
Yamakagashi venom, which acts as a prothrombin activator, exhibits strong blood
coagulation activity and a weak thrombin-like effect,48 leading to DIC with a fibrinolytic phenotype7(Table
2).
Yamakagashi antivenom is derived from an equine source and is used as an off-label drug
in Japan.49 Therefore, clinicians are
required to use it in the context of clinical research. Over a period of 40 years, Hifumi
et al. conducted a retrospective survey of 34 patients, 19 of whom were treated with
antivenom.50 The authors found no
significant differences in baseline characteristics and laboratory data between those
treated and not treated with yamakagashi antivenom. However, hospital mortality was
significantly reduced among patients treated with yamakagashi antivenom (0% vs. 26.7%
without antivenom; P = 0.03). Moreover, the number of patients with renal
failure who required hemodialysis was significantly lower among those treated with
yamakagashi antivenom (5.3% vs. 40.0% without antivenom; P = 0.03).
Therefore, antivenom is considered to be an effective treatment for yamakagashi bites.
Fibrinogen levels <100 mg/dL are considered to be an appropriate indicator for
antivenom administration in clinical practice.13,49,51
Yamakagashi antivenom was manufactured via the immunization of rabbits in 1986 and of
goats in 1987. However, low supply levels recently led to the immunization of horses, a
practice that was supported by Health Science Grants (1998–1999) from the Ministry of
Health, Labor, and Welfare in 2000.49
The fact that more than 16 years have passed since the most recent round of antivenom
production is of great concern. Although our research group has examined the potency and
quality of this antivenom, we cannot guarantee its quality in the future.
Redback spider (Latrodectus hasselti) bites
Since the first case reported in Osaka in 1997, redback spider bites have been a clinical
and administrative issue in Japan.11 The adult female redback is characterized
by a spherical black body (approximately 10 mm long) with a prominent red stripe on the
upper side of the abdomen and a red streak on the underside (Fig. 3). Alpha-latrotoxin, the main toxin produced by the redback
spider, causes synaptic vesicle exocytosis from the presynaptic terminal via a
calcium-dependent mechanism, leading to the release of catecholamines and
acetylcholine.11
Currently, two types of redback spider antivenom exist; these are produced by the
Commonwealth Serum Laboratories in Australia and by our research group in Japan.11,12 Because these antivenoms are used as off-label drugs in
Japan, clinicians are required to join a clinical research group to use either of the
antivenoms in clinical practice.11
To date, fatalities related to redback antivenom have not been reported in Australia
since the development of antivenom.52 In
2014, Isbister et al. conducted a RCT to evaluate the effect of redback antivenom, and
concluded that the addition of antivenom to standardized analgesia in patients with
latrodectism did not significantly improve pain or systemic effects.53 However, that study has raised some
concerns. In Australian emergency departments, some patients with redback spider bites,
including children, pregnant women, and the elderly, have increased risks of developing
severe or systemic symptoms and are more likely to receive antivenom.54 However, children, pregnant women, and the
elderly were not included in the abovementioned target study population.
In 2013, the Ministry of Health, Labor, and Welfare of Japan established a research group
to evaluate the safety and efficacy of antivenom and to organize and maintain information
about redback spider bites. Our research group conducted a 5-year retrospective study to
elucidate the clinical characteristics of these bites and clarify the therapeutic efficacy
of antivenom. Our survey evaluated the efficacy of antivenom in a small number of
patients, including children and the elderly. In addition, we carefully discussed the
domestic production of redback spider antivenom, which thereafter was completed in
December 2015. According to this study, the routine use of antivenom for redback spider
bites is not recommended; however, the efficacy of antivenom for the treatment of patients
in the above-mentioned high-risk group should be evaluated further. We further note that
redback spider antivenom protects against toxicity from widow spider venom, and therefore
could be useful as a preventive measure in the event of a pandemic of widow
spiders.55,56