Lymphatic Imaging
The lymphatic system is made up of the lymphatic organs (lymph nodes, spleen, thymus,
tonsils, and appendix) and the vessels (lymph capillaries, precollectors, collectors,
trunks, and thoracic ducts). When the lymphatic pathway is impaired, lymphatic leakage may
cause lymphoceles, chylothorax, or chylous ascites, and a lymphatic obstruction can result
in lymphedema in the extremities. Consequently, lymphatic imaging is indicated to obtain
anatomical information for accurate diagnosis and treatment planning. Particularly for
lymphedema, the advent of new microsurgical approaches, such as lymphaticovenular
anastomoses (LVAs) to bypass the excess fluid component by joining with the circulatory
system peripherally, in addition to conventional conservative therapies, has underscored the
importance of lymphatic imaging. For the correct evaluation of the function and pathways of
impaired lymphatics, various imaging modalities can detect lymphatic flow, which is often
masked beneath the dermal backflow (DBF) caused by the accumulation of lymph in either the
skin or subcutaneous tissues.16,17 In
healthy individuals, the “linear pattern” of lymphatic channels can be seen (Fig. 1A). However, the DBF observed in lymphedema
patients often obscures the lymphatic vessel pathways toward the proximal regions (Fig. 1D).

Because direct lymphangiography, which requires a skin incision for the insertion of a
catheter into a lymphatic vessel, is so invasive,19,20
indirect lymphography with an intradermal or subcutaneous injection of contrast agent is
currently the most often used method of lymphatic imaging. Representative imaging modalities
include lymphoscintigraphy,21 magnetic
resonance lymphography (MRL),22,23,24 and
indocyanine green (ICG) near-infrared fluorescence (NIRF) lymphography (Fig. 1A,D).5,6,25,26
Additionally, non-contrast MRL27,28 and
high-resolution ultrasound (US) imaging29,30,31,32 have been
introduced as new techniques without the need for contrast agent injection, which can cause
adverse reactions in some patients. Inevitably, all these imaging modalities are based on
different principles; consequently, every option has specific advantages and
disadvantages.19 Moreover, these
imaging approaches lack standardized procedures even within centers that specialize in
lymphatic disorders, resulting in variable results.33 Furthermore, none of these methods can visualize the anatomical
architecture of the small veins around the peripheral lymphatics19 or the actual flow of lymphatic transport within a lymphatic
vessel, both of which have long been unmet needs in the field of lymphatic surgery to
achieve more successful LVA.
Unlike previous techniques, PAI has a high spatial resolution with an acoustic depth of
penetration. The spatial resolution of PAI varies from the submicrometer range at
submillimeter imaging depths to the submillimeter range at depths up to several
centimeters.34 Over these ranges, PAI
provides detailed images of the superficial blood vessels containing hemoglobin. Using an
exogenous contrast agent such as ICG, lymphatic vessels can also be visualized clearly. The
unique characteristics of PAI can therefore improve the quality of research in this
field.
Photoacoustic Imaging
PAI is based on the photoacoustic (PA) effect, first described by Alexander Graham Bell in
1880,35 which occurs when light
illuminates tissues. When a tissue is illuminated with short-pulse non-ionizing light,
absorption of the optical energy by local molecules causes the local temperature to
increase, resulting in transient thermoelastic expansion. This expansion generates localized
pressure waves (ultrasound) that can be detected using ultrasonic transducers to generate an
image.36 Representative
light-absorbing biomolecules include oxy- and deoxyhemoglobin, lipids, water, and melanin.
These are endogenous chromophores, and each exhibits its own characteristic absorption
spectrum. For example, in the detection of PA waves from hemoglobin illuminated by
near-infrared (NIR) light, blood vessels can be visualized without using exogenous contrast
agents.37,38,39,40,41,42,43,44,45,46 By
utilizing multiple wavelengths of illumination, PAI can differentiate arteries from veins by
assessing the oxygen saturation of the blood thanks to the difference in the absorption
profiles of oxyhemoglobin and deoxyhemoglobin.7,37,47,48 In
addition to the spectral unmixing of chromophores, the unique scalability of the spatial
resolution and depth penetration resulting from the combination of light and sound with PAI
also highlights important advantages over conventional imaging techniques. Therefore, PAI
provides not only structural but also functional information from molecules in real-time at
clinically relevant depths with a relatively high spatial resolution and without the use of
ionizing radiation.7 Moreover, because the
transducers can be arranged in two dimensions (2D) or three dimensions (3D), either a 2D
cross-sectional image or a 3D volumetric image can be reconstructed. Utilizing the
information provided by PAI, many clinical applications have been demonstrated
recently.47 Although PAI is still an
emerging technology, a few commercial PAI systems have already been approved for clinical
use by regulatory authorities in the European Union.47 In addition to commercialized clinical and preclinical systems, most of
which are equipped with handheld PA probes,8,9,49,50 many
different PAI-platforms, including laboratory prototypes, also exist. PA microscopy,
intravascular PAI via catheters, PA endoscopy, and PA tomography (PAT) with a stationary
examination bed unit are some examples. The wide range of preclinical and clinical
applications using these systems has been reviewed elsewhere.7,36,47,51
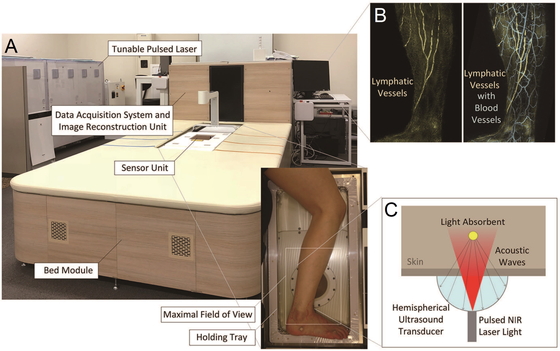
Recently, a prototype PAT system with a wide field of view (WF-PAT) has been developed by a
Japanese research group (Fig.
2).38 This system
has metamorphosed through several versions37,39,40,41 to
acquire PA signals from a maximal field of view (FOV) of 270 × 180 mm2 in 10 min
with a resolution of approximately 0.2 mm.38 Using this type of system, various clinical studies have been performed.
Observation of the peritumoral and intratumoral vasculature, the response to
chemotherapy,41 the investigation of
potential biomarkers42 related to breast
cancer, the evaluation and preoperative mapping of the 3D vasculature of the thigh for free
flap reconstruction surgery,43,44 and
analysis of the findings in digital or palmar arteries related to motion,45 aging,46 or inflammatory disease (psoriasis)48 have shown encouraging results.
Photoacoustic Lymphangiography
PAL is a new imaging technique that is being investigated clinically to visualize the
lymphatic vessels using PAI technology.8,9,10,11,12,13,14,15 Because
lymphatic fluid is transparent, the lymphatic vessels lack endogenous chromophores to absorb
light in the NIR wavelength range, with which a deeper penetration of light is achieved due
to its lowest total absorbance in the background tissue components. As a result, exogenous
imaging agents such as ICG8,9,10,11,12,13,14,15 or
methylene blue49,52 have been used to facilitate imaging. This
approach enables PAL not only to visualize both lymphatic vessels and small veins
simultaneously but also to spectroscopically distinguish between them using the difference
in absorption spectra between the dye taken up by the lymphatics and the hemoglobin in the
veins.12 This feature allows visual
differentiation of lymphatics from blood vessels using color to help operators distinguish
them.8,9,10,11,12,13,14,15,52 This is
an important advantage over traditional medical imaging modalities that give each coordinate
a single value and therefore produce only monochromic images, often leading to the lymphatic
vessels being misidentified as small veins. PAL can also provide real-time imaging of the
lymphatic vessels, which is useful for direct observation of the lymphatic pumps.8,10,11 The
pumps involve spontaneous smooth muscle contraction of the collecting lymph
vessels53 to generate a flow of
lymphatic fluids, which may reflect each vessel’s capacity for lymph transport.54
Two kinds of preclinical commercial devices with handheld probes have been used to identify
the lymphatic vessels in a healthy person9
and in lymphedema patients.8 However, the
FOV was so limited that lymphatic and vascular mapping over a large area of the limbs was
not possible. In contrast, PAL using the WF-PAT system38 (WF-PAL) revealed previously unknown 3D structural information over a
large area in both healthy and lymphedematous extremities.10,11,12,13,14,15
Lymphatic vessels in healthy people
In PAL, ICG is so frequently used as a contrast agent that NIRF lymphography is often
undertaken at the same time.8,12,13 Because
ICG contains trace amounts of iodine, administration to subjects with previously known
iodine reactivity should be avoided. Whereas NIRF shows the typical linear courses of
lymphatic vessels under healthy conditions, the deeper lymphatic vessels become blurred
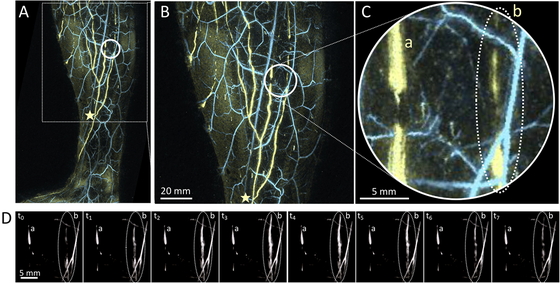
with this technique (Fig. 1A). WF-PAL, however,
visualizes the corresponding lymphatic vessels more clearly compared to those visualized
by NIRF, in 3D (Fig. 1A, B).12 Furthermore, the superficial venous network
around the lymphatics, which may not be visualized by NIRF, can also be depicted (Fig. 1C).12
The WF-PAT system can perform imaging in still mode, in which a large area can be imaged
by scanning with a hemispherical US detector array, as utilized for WF-PAL. Additionally,
the system can operate in video mode, in which a specific site with a FOV of 20 mm in
diameter can be irradiated with laser light to repeatedly obtain updated PA images of the
same site,25 thereby potentially
enabling real-time visualization of the lymphatic pumps10,11 (Fig. 3; a supplementary
video is also available). The lymphatic pumps observed using this function occurred
intermittently at various intervals, and the velocity of the lymphatic flow also varied
from subject to subject. However, there was a tendency for the flow in the upper limbs to
be faster than that in the lower limbs.10
Abnormal lymphatic vessels in lymphedema patients
In lymphedema patients (e.g., as shown in Fig.
4A), particularly those with a distinct DBF on lymphoscintigraphy14 or NIRF12 (Fig. 1D, 4B), WF-PAL can
reveal the complex 3D structures of the DBF in high resolution10,11,12,14,15 (Fig. 1E, 4D). Visualization of the lymphatics that
generate a DBF had never been achieved at such a resolution before the development of
WF-PAL.14 In a previous study using
computed tomography–lymphography (CT-LG), which showed the 3D architecture of a
DBF,17 the small lymphatic vessels
branching upward from the deep lymphatic collectors toward the dermis were visualized.
However, the complex 3D structure of the DBF itself, as shown with WF-PAL, was not
possible due to limited sensitivity20
and resolution. The smallest lymphatic vessels identified by CT-LG and PAL were
0.717 and 0.28,11 mm in diameter, respectively. On the other hand, other 3D
imaging modalities, including MRL22,23,24 and
single photon emission CT (SPECT-CT),55
depict DBFs as a blurred area on the skin, which limits the visualization of the lymphatic
vessels inside the DBF itself.
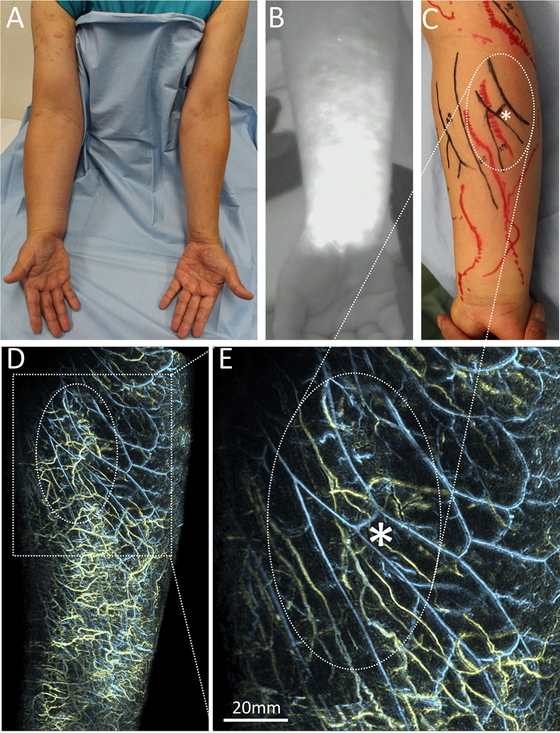
PAL also showed that there were many collecting vessels underneath the DBF and many of
these seemed to be twisted (Fig. 4E), which may
reflect the lymphatic overload and increased internal pressure. A previous histochemical
study revealed that as lymphedema progresses, the lumen of lymphatic vessels become
dilated, then narrowed, and then finally obstructed.56 If the morphological features of the lymphatic vessels visualized
noninvasively by PAL follow this process, then progression of the pathological changes of
each vessel may be predicted, which will be very useful for selecting target lymphatic
vessels for LVA.
Advantages for clinical applications toward the better management of
lymphedema
Whereas other imaging modalities such as lymphoscintigraphy and NIRF lymphography are
unable to visualize the lymphatic vessels underneath a DBF,21 PAL has successfully identified not only the lymphatic
vessels, but also the small veins underneath a DBF8,11 (Fig. 4E). Contrast-enhanced MRL also obtains
full-thickness 3D information on the lymphatic vessels and soft tissue in a DBF23; however, it does not provide information on
the relationship between the lymphatics and small veins. Recently, conventional
high-frequency US (CHFUS) with an upper frequency of 15–24 MHz29,30,31 and
ultrahigh-frequency US (UHFUS) with an upper frequency of 70 MHz32 were used to visualize the lymphatic vessels underneath a
DBF as seen by NIRF. However, these imaging procedures can be difficult for less
experienced operators, in part because the monochromic 2D image makes it challenging to
distinguish lymphatic vessels from small veins or nerves. In PAL, the lymphatic and blood
vessels can be differentiated by color8,10,11,12,13,14,15,52(Fig. 1C,F; 3A-C; 4D,E), rendering the images easier
to interpret even for individuals without medical knowledge.
Another advantage of WF-PAL is that it generates information on the precise structure of
small veins. Although veins are an important counterpart to lymphatic vessels for a
successful LVA,57 there has never been a
tool for mapping superficial veins at the submillimeter scale.58 Because PAL can clearly visualize vessels as small as 0.2 mm
in diameter8,11 in superficial regions up to 20 mm in
depth,14 the resultant morphology of
the vasculatures is similar to that marked on the patient as part of the planning of LVA
surgery using conventional methods such as NIRF for the lymphatics and CHFUS for the small
veins (Fig. 4C,E). Whereas the conventional
procedures for this study took more than 60 min for mapping by an experienced examiner
(SH) using NIRF and CHFUS, WF-PAL took approximately 15 min to acquire each
image.12
Additionally, although the feasibility of PAL for LVA surgery has already been indicated
by comparing the vessel position based on PAL with the intraoperative surgical microscopic
view,8 WF-PAL also provides
information on the 3D relationship between the lymphatic and venous pathways over a wide
area, which was not previously acquired using other imaging techniques. Therefore, WF-PAL
enables improved LVA planning with the choice of better target veins to increase the
drainage of lymph into the local venous circulation by taking into account the 3D
relationship between the lymphatic vessels and the functional perforating veins to achieve
more effective lymphatic drainage.
Moreover, the outstanding features of PAL allow postoperative assessment of anastomoses
because PAL provides a clear image to visualize both the lymphatic vessels and the veins.
No conventional modality has succeeded in imaging the anastomosis itself. Although
evaluation of the postoperative patency rate is an important outcome of LVA surgery, there
is no ideal method to assess the patency of LVAs in the clinical setting.59 In two clinical studies that used NIRF to
assess patency,25,26 no more than half of the anastomoses could
be assessed because of depth limitations. In contrast, PAL can clearly visualize vessels
in superficial regions up to 20 mm deep8,14 and
those above the deep fascia.12Therefore,
it should be possible to visualize the anastomoses directly because LVA is usually
achieved between vessels in the superficial layers.29,30,31,57
Limitations and future directions
PAI is still an emerging technology currently under development, and, in addition to the
major advantages mentioned above, there are still some important challenges to
overcome.7,47 First, given the limitations of light
penetration, PAI may result in poor image quality in areas with thicker subcutaneous
tissues,7 which are often found in
lymphedema patients. Also, the spatial resolution will be high at higher US frequencies,
but with lower depth penetration as a trade-off because of the increasing attenuation of
ultrasound with increasing frequency.7,36 This is
similar to the finding that the deepest layer from which UHFUS can obtain images is 10 mm
from the superficial surface.33
Furthermore, the difficulty in detecting vessels deeper than the deep fascia,12,15,43 which cannot be explained using the principles above, may be due to
acoustic heterogeneity.60 The
differences in sound velocity in tissues such as subcutaneous tissues, deep fascia, and
subfascial tissues can hinder the reconstruction of a clear image from the intensity of
the PA signals. Therefore, the implementation of compensation algorithms to correct for
the distribution of sound velocities in different tissues61 as part of the image reconstruction process may improve the
image quality.
Second, the signal intensity generated by hair shafts is stronger than that of blood
vessels or ICG-filled lymphatic vessels; the reason for this is that melanin provides
great contrast for PAI in the NIR wavelength range often used for vascular
imaging.7 Even if hairs are removed
using hair clippers before an examination, residual hair roots can interfere with analysis
of the images.8,38 The application of depilatory creams to
completely remove the hair shaft in advance may be an option; however, implementation of a
body surface detection algorithm62 may
help to remove the hair volume data and facilitate the analysis of deeper structures.
Regarding WF-PAT, in addition to the common limitations noted above, this modality cannot
obtain structural information other than that from the targeted chromophores in tissues
such as the dermis, fat, superficial and deep facias, vessel walls, or nerves. However,
such additional tissues could be visualized by systems that integrate PA and US
imaging.50 Information on vessel
wall thickness may be important for understanding the pathophysiological state of
lymphedema31,56 or atherosclerotic diseases.7
Another limitation is a limited FOV. Although WF-PAT has a relatively large FOV among PAI
devices, its configuration with a shallow holding tray38 limits the body regions that can be imaged. Because lymphatic
surgeons need to know the lymphatic pathways throughout the limbs to assess and plan
surgery for lymphedema, the use of PAL in combination with other imaging modalities,
including lymphoscintigraphy, MRL, or NIRF lymphography, may be necessary to make accurate
decisions and achieve good clinical outcomes.
Currently, the best potential application of PAL is for planning LVA procedures; however,
the identification of target vessels in clinical practice can be difficult. Although the
accuracy of lymphatic and venous mapping using WF-PAL imaging has not been clinically
assessed, it may be important to carefully reproduce the patient’s positioning between the
imaging examination and surgery. Vascular mapping technology on the body using projection
mapping44,63 or augmented reality64,65 may also be useful for the preoperative preparation of LVA
surgeries.
Nevertheless, as this rapidly progressing technology improves further, the current
limitations may be overcome, paving the way for the clinical use of PAL, which it is hoped
will contribute to improved treatment for lymphedema patients.