抄録
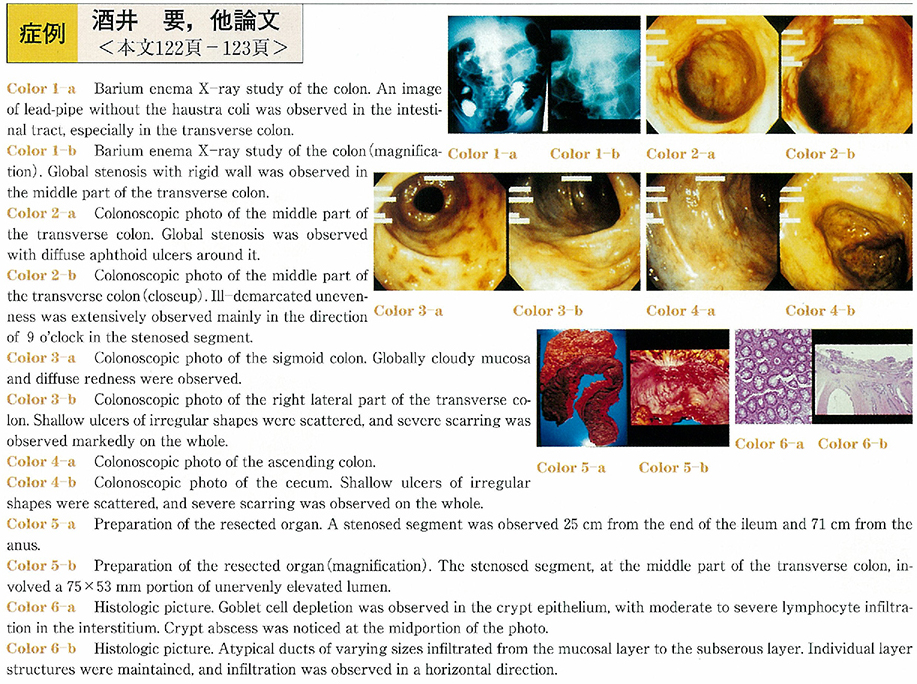
The patient was a 46-year-old male. He was innately healthy, but noticed blood in stool and received a first colonoscopic examination in March, 2003. Colonoscopy showed almost normal mucosa in the rectum. It aolso exihibited almost normal mucosa in the sigmoid colon, only diffuse aphtha was seen. Severe fibrosis was markedly observed from the descending colon to the ileocecum, and relatively shallow ulcers of irregular shapes were scatterd in places. In addition, moderate stenosis was detected in the middle part of the transverse colon. It was difficult to make an endoscopic diagnosis because the stenosis was ill-demarcated with no appreciable elevated or depressed lesions. A biopsy of the stenosed segment revealed a well-differentiated adenocarcinoma. In contrast, the surrounding ulcerated part was found by biopsy to be ulcerative colitis.
Subsequently, total colectomy was performed, and the final pathological diagnosis was type 5 large intestine cancer associated with ulcerative colitis. It has recently been reported that large intestine cancer in ulcerative colitis patients is detected frequently at 7 to 8 years or more on average after initial onset. This case was very rare since the advanced cancer was detected by the first endoscopic examination, while no symptoms suggestive of ulcerative colitis were noted during the course. Therefore, our experience is reported here with some discussion.