症例
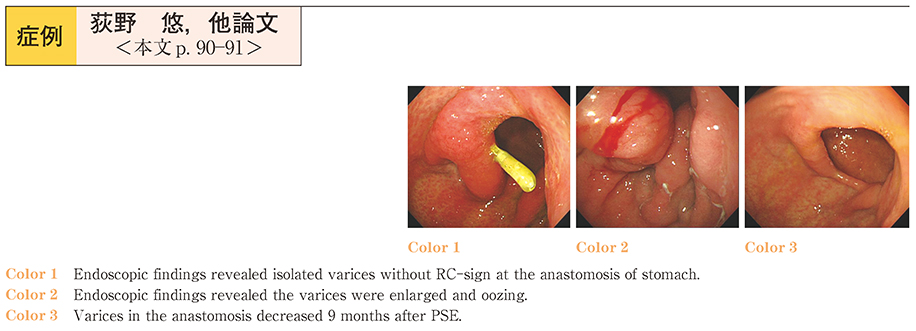
部分的脾動脈塞栓術が著効した左側門脈圧亢進症性胃静脈瘤出血の1例
荻野 悠, 三村 亨彦, 土方 一範, 馬越 智子, 乾山 光子, 岸本 有為, 伊藤 謙, 岡野 直樹, 中野 茂, 五十嵐 良典
著者情報
-
荻野 悠
東邦大学医療センター大森病院/消化器内科
-
三村 亨彦
東邦大学医療センター大森病院/消化器内科
-
土方 一範
東邦大学医療センター大森病院/消化器内科
-
馬越 智子
東邦大学医療センター大森病院/消化器内科
-
乾山 光子
東邦大学医療センター大森病院/消化器内科
-
岸本 有為
東邦大学医療センター大森病院/消化器内科
-
伊藤 謙
東邦大学医療センター大森病院/消化器内科
-
岡野 直樹
東邦大学医療センター大森病院/消化器内科
-
中野 茂
東邦大学医療センター大森病院/消化器内科
-
五十嵐 良典
東邦大学医療センター大森病院/消化器内科
ジャーナル
フリー
2014 年 84 巻 1 号 p. 90-91
詳細
- 発行日: 2014/06/14 受付日: - J-STAGE公開日: 2014/06/21 受理日: - 早期公開日: - 改訂日: -
PDFをダウンロード (564K)
メタデータをダウンロード
RIS形式
BIB TEX形式
テキスト
メタデータのダウンロード方法
発行機関連絡先
(EndNote、Reference Manager、ProCite、RefWorksとの互換性あり)
(BibDesk、LaTeXとの互換性あり)