2017 Volume 242 Issue 2 Pages 115-120
2017 Volume 242 Issue 2 Pages 115-120
Osteogenesis imperfecta (OI) is an inherited bone disorder that causes fractures due to impaired production of collagen type I. In recent years, denosumab, a human monoclonal antibody against receptor activator of nuclear factor κB ligand (RANKL), has become widely used as an anti-osteoclastic agent for osteoporosis. This study investigated osteoporotic cases of OI to examine effects of denosumab on bone fragility. This was a retrospective, consecutive case series that included 3 female patients aged 42, 40, and 14 years, respectively. One patient carries a point mutation (c.G769A) in the COL1A1 gene, encoding collagen type I alpha 1 chain, which causes an amino-acid substitution (p.G257R). By contrast, no mutation was found in the analyzed regions of the OI responsive genes in another two patients (mother and daughter). These three patients underwent subcutaneous injection of denosumab every 6 months. All patients underwent dual-energy X-ray absorptiometry for bone mineral density (BMD) measurement of the lumbar 1-4 spine (L-BMD) and bilateral hips (H-BMD) before and during treatment. BMD and laboratory data were evaluated before, between 2 and 4 months, and at 6, 12, 18, and 24 months of therapy. No fractures or severe side effects, such as hypocalcemia, were observed during denosumab treatment. Both L-BMD and H-BMD were increased by denosumab. At 24 months, the mean percentage changes in L-BMD and H-BMD were 14.7% and 15.1%, respectively. In conclusion, no bone fragility fractures occurred during 2 years of denosumab administration in OI patients. Denosumab therefore is a good therapeutic option in the OI patients.
Osteogenesis imperfecta (OI) is an inherited disease that causes fractures, skeletal deformities, scoliosis, and reduced bone mass due in most cases to impaired production of collagen type I (Rauch and Glorieux 2004). OI is a rare disorder (1 in 15-20,000 births) (Forlino and Marini 2016) of the connective tissue that has major manifestations in bone, leading to skeletal fragility and substantial growth deficiency (Marini et al. 2007). The loss of cartilage-associated protein (CRTAP), which is required for post-translational prolyl 3-hydroxylation of collagen, was first identified as a disease-causing gene of OI in 2006 (Barnes et al. 2006; Morello et al. 2006). A widely used clinical classification of OI was proposed in 1979 (Sillence et al. 1979) and later revised by Van Dijk and Sillence in 2014 (Van Dijk and Sillence 2014). Among OI subtypes, type I is relatively mild and the most common. Type II OI causes death in the perinatal period, while type III OI results in obvious bone deformities and short stature due to frequent fractures.
Even in type I OI, it is important to treat bone fragility in OI to reduce the risk of severe fractures that deteriorate patient quality of life and activities of daily living. The most commonly prescribed medications for OI are intravenous bisphosphonates (BPs) (Glorieux et al. 1998; Semler et al. 2011), although their effects have been limited to only modest reductions in the incidence of fractures (Land et al. 2007). In a clinical trial of the BP risedronate for OI, the mean increase in lumbar bone mineral density after 1 year was 16.3%, but clinical fractures had occurred in 29 (31%) of 94 patients. At 2 years, clinical fractures had been recorded in 46 (53%) of 87 patients (Bishop et al. 2013).
In recent years, denosumab has become widely used for primary and secondary osteoporosis. Denosumab is a fully human monoclonal antibody to receptor activator of nuclear factor κB ligand (RANKL) that blocks its binding to RANK (Fazil et al. 2015). Through the inhibition of RANKL, the drug has been shown to decrease bone resorption, increase BMD, and reduce the risk of fractures in postmenopausal women with osteoporosis (Lewiecki et al. 2007; Bone et al. 2011; McClung et al. 2012). Denosumab is a useful drug even in BP-unresponsive primary osteoporosis as well (Kamimura et al. 2017). Recently, denosumab has been used for bone fragility even in children with OI by several research groups (Semler et al. 2012; Hoyer-Kuhn et al. 2014, 2016). However, the detailed efficacy and adverse effects of denosumab in OI are uncertain.
This study retrospectively investigated 3 patients with OI to clarify the utility of denosumab on bone fragility in osteoporotic OI patients and discuss available treatments.
Three female patients were diagnosed as having OI by 2 doctors with genetic counseling certification and began treatment with denosumab for bone fragility. All 3 patients had osteoporosis that met the revised criteria established by the Japanese Society of Bone and Mineral Research (Orimo et al. 2001) and had experienced multiple fractures before denosumab therapy. Characteristics of the patients are summarized in Table 1. The frequency of fractures was 10 or more times in 2 patients (Patient 1 and 2), and 7 times in Patient 3, a daughter of Patient 2. Genetic analyses revealed a missense mutation in the COL1A1 gene, encoding collagen type I alpha 1 chain, in Patient 1, while no mutation was found in the analyzed regions of the OI responsive genes in Patient 2 and 3. Patient 1 has no family history. The type of OI according to Sillence’s classification was type Ia in all patients. This type is characterized by blue sclerae, premature deafness, mild to moderate bone fragility, and normal teeth. All of them do not suffer from deafness. Denosumab was injected subcutaneously every 6 months (i.e., at 0, 6, 12, 18, and 24 months).

Patient characteristics.
OI, osteogenesis imperfect; BMI, body mass index; SD, standard deviation; BP, bisphosphonate; Ca, calcium; Mg, magnesium.
All subjects underwent dual-energy X-ray absorption (DXA) fan-beam bone densitometry (Lunar Prodigy; GE Healthcare Bio-Sciences Corp., Piscataway, NJ) at the lumbar 1-4 levels of the posteroanterior spine [L-BMD (g/cm²)] and bilateral hips [H-BMD (g/cm²)] before and during administration. The coefficients of variation (CVs) of the BMD measurements at the lumbar spine and hip were 0.7% and 1.1%, respectively (Uchiyama et al. 2015).
Analysis of laboratory dataAs a bone formation marker, bone alkaline phosphatase (BAP) (μg/L) was measured by a chemiluminescent enzyme immunoassay. Urinary N-terminal telopeptide of type-I collagen (NTX) (nmol BCE/mmol Cr) and tartrate-resistant acid phosphatase 5b (TRACP-5b) (mU/dL) were assessed by an enzyme-linked immunosorbent assay (ELISA), as markers of bone resorption. 1,25 (OH)2D (ng/mL) and parathyroid hormone (PTH) (pg/mL) were determined by an immunoradiometric assay. After overnight fasting and omission of the first morning samples, serum and urine were collected between 8:30 a.m. and 11:00 a.m. Immunoassays were performed by SRL Inc. (Tokyo, Japan). The BMD and laboratory data were basically evaluated before, between 2 and 4 months, and at 6, 12, 18, and 24 months of denosumab administration. Data were analyzed by means of paired t-test using SPSS software version 21 (SPSS Japan Inc., IBM, Tokyo, Japan). The level of significance was set at P < 0.05.
This investigation was approved by the Institutional Ethical Review Board of Shinshu University School of Medicine, Japan, prior to its commencement. Written informed consent was obtained from all subjects. Study methods were carried out in accordance with the approved guidelines.
Both L-BMD and H-BMD were increased in all cases (Fig. 1). Electrolyte data are presented in Table 2. Serum calcium levels during denosumab administration were stable in the cohort, with no subsequent hypercalcemia that is frequently observed after denosumab administration as rebound inhibition of bone resorption. No severe adverse effects were observed in this study.
The radiological and laboratory findings are respectively summarized in Tables 3 and 4. No patient suffered a fracture during denosumab administration for 2 years.
In Patient 2 and 3, bone metabolism was strongly suppressed by denosumab administration and 1,25 (OH)2D was increased at 1 month of administration (Fig. 2). In Patient 1, BAP, TRACP-5b, and NTX all temporarily increased and 1,25 (OH)2D transiently decreased.

Changes in BMD before and during denosumab administration.
Both lumbar BMD and hip BMD were increased at 2 years of drug administration.
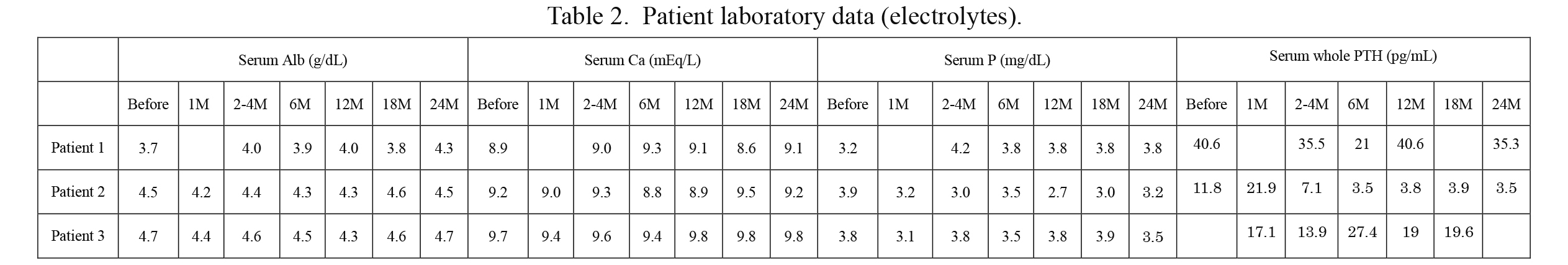
Patient laboratory data (electrolytes).
Alb, albumin; Ca, calcium; P, phosphorus; PTH, parathyroid hormone; M, months.
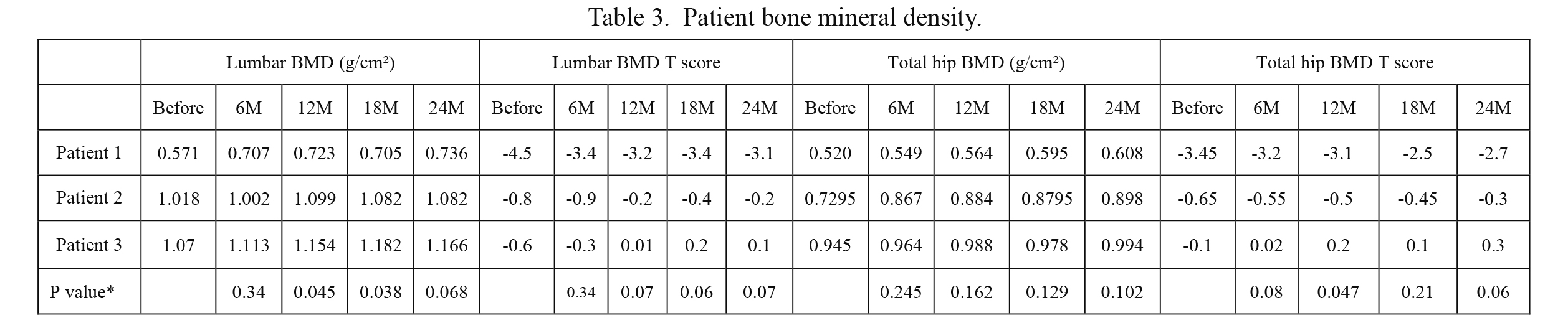
Patient bone mineral density.
BMI, body mass index; BMD, bone mineral density; M, months.
*Compared with pre-treatment value.

Patient laboratory data (bone metabolism markers).
BAP, bone-specific alkaline phosphatase; NTX, type I collagen amino-terminal telopeptide; TRACP-5b, tartrate-resistant acid phosphatase 5b; 1,25(OH)2D, 1-alpha, 25-dihydroxyvitamin D; M, months; N/A, not available.
*Compared with pre-treatment value.

Changes in bone turnover markers before and during denosumab administration.
(a) The bone formation marker BAP was decreased at the final follow-up. (b, c) The bone resorption markers urinary NTX and TRACP-5b were largely decreased at the final follow-up. (d) 1,25(OH)2D was not remarkably changed at the final follow-up.
Patient 1 (Adult patient): A 42-year-old female was diagnosed as having OI type Ia and found to carry a point mutation (c.G769A) in the COL1A1 gene, which cause an amino-acid substitution at position 257 (p.G257R). She had suffered more than 10 fractures before denosumab administration and her most recent fracture had occurred 3 months prior to treatment. She had not been taking medication for fracture prevention. No fractures occurred over the 2 years of denosumab treatment. Her L-BMD and H-BMD respectively improved from 0.571 and 0.520 before treatment to 0.736 (28.9% increase) and 0.608 (16.9% increase) at 2 years of treatment. Bone metabolism markers temporarily increased during the treatment course.
Patient 2 (Adult patient): A 40-year-old female was clinically diagnosed as having OI type Ia. She had suffered more than 10 fractures before denosumab administration and her most recent fracture had occurred 1 year prior to treatment. She had not received BPs before denosumab. No fractures occurred over the 2 years of denosumab treatment. Her L-BMD and H-BMD respectively improved from 1.018 and 0.730 before treatment to 1.082 (6.3% increase) and 0.898 (23.1% increase) at 2 years of treatment.
Patient 3 (Adolescent patient): A 14-year-old female was clinical diagnosed as having OI type Ia. She had suffered 7 fractures before denosumab administration and her most recent fracture had occurred 1 year prior to treatment. She had received BPs for 2 years before denosumab (see Table 1), but her incidence of fractures did not decrease. No fractures occurred over the 2 years of denosumab treatment. Her L-BMD and H-BMD respectively improved from 1.07 and 0.945 before treatment to 1.166 (9.0% increase) and 0.994 (5.1% increase) at 2 years of treatment.
This retrospective study is the first treatment report of denosumab for osteoporotic OI patients in Japan. Since Patient 1 and 2 suffered from repeated fractures, denosumab was selected as first therapeutic modality, and Patient 3 has previously been treated with bisphosphonates and switch to denosumab due to the poor response. In all 3 patients, bone density increased and bone fracture did not occur during the 2-year study period.
As osteoporosis develops in the majority of patients with OI (Van Dijk and Sillence 2014), adequate treatment of bone fragility is paramount in these individuals. The low bone mass in OI is caused not by a lack of bone formation activity, but rather by high bone resorption. Until now, patients with severe clinical OI symptoms have been treated with pamidronate, neridronate, and other intravenous BPs (Glorieux et al. 1998; Semler et al. 2011). However, skeletal symptoms sometimes show a poor response to BPs (Land et al. 2007).
Fractures in OI patients chiefly occur from childhood to puberty (Major et al. 2008). In Patient 3, the patient’s height increased from 159 cm to 161 cm after 2 years, indicating that she was still growing. Fractures had earlier persisted in the girl despite BP administration. The remaining cases experienced repeated fractures in spite of reaching adulthood. Since no patient experienced a fracture during denosumab treatment in this study, the drug may be useful in OI patients possessing a high fracture risk. In the Patient 3, the treatment started at the end of growth which is time when fracture rate decrease in most of the patients. Therefore, it is unlikely that the fracture free interval was caused by only the denosumab treatment in this patient.
The change of BMD during treatmentIn our series, BMD increased soon after denosumab administration and remained improved for up to 2 years. Patient 2 and 3 had relatively high baseline BMD but suffered repeated fractures before treatment. In addition to fracture prevention, there is also the possibility of an improvement in bone quality by denosumab. The modest increase in BMD in our cohort was thought to have resulted from the originally high BMD values.
The change of bone turnover markers during treatmentBone formation and bone resorption markers were both generally improved by denosumab injection in this study, in agreement with other report (Nakamura et al. 2015). The changes in bone turnover markers during denosumab administration were comparable among our OI patients except Patient 1. The cause of elevated BAP and TRACP-5b in Patient 1 was unknown.
The effect of denosumab on growth in childrenThere are no published clinical reports on the effect of denosumab on growth in children, nor have the growth effects of RANKL inhibition been determined. Histological studies have suggested that the influence of denosumab on linear growth was not significant (Wang et al. 2014). In our adolescent case (Patient 3), no apparent growth disturbance was observed; her height increased from 159 cm at the first administration to 161 cm after 2 years and she was within the normal age-based height range. Denosumab may therefore be considered for adolescent cases as well.
The differences of treatment effect between children and adultBone metabolic characteristics are different in adults and children, before and after growth plate closure. The change of BMD increase in adolescent case was relatively low, although her BMD increased and bone fracture did not occur after the treatment. There was no certain difference between adults and children regarding the changes of turnover markers in those series.
Our cohort had experienced multiple fractures before denosumab treatment, but no such incidents were recorded over the 2-year administration period. These findings suggest that denosumab has strong preventative effects on fracture in OI patients in addition to a BMD increase, although the mechanism of fracture prevention by denosumab requires further consideration. Since denosumab discontinuation causes a marked decrease in BMD (Miller et al. 2008; Bone et al. 2011), BPs and other alternative treatments are advised after its discontinuation.
In this study, no bone fragility fractures occurred over denosumab administration for 2 years. Denosumab therefore represents a strong drug candidate for OI patients having a high risk of fracture.
LimitationsThe limitations of the current study include the lack of a control group, small sample size, wide age range, and retrospective design. Nonetheless, our series provided evidence of a good response in BMD after 2 years of denosumab treatment in the rare disease OI.
This study is the first treatment report of denosumab for osteoporotic OI patients in Japan. Denosumab treatment causes good responses in BMD and bone turnover markers in osteoporotic OI patients and represents an effective treatment option for OI.
Y.N. directed this study. T.S. collected patient data. M.U., and Y.N. wrote the main manuscript. J.T., M.K., S.I., S.U., and H.K. gave suggestions on this study. T.Y. and T.K. performed genetic analyses in this study. All authors reviewed and approved the manuscript.
We thank Mr. Trevor Ralph for his English editorial assistance.
The authors declare no conflict of interest.