Introduction: Solitary fibrous tumor (SFT) that mainly arise in the pleura, is rarely occurs in the spinal canal. Until now, 41 cases of SFTs arised in the spinal canal have been reported, 16 cases of which were intramedullary SFTs. Here, we reported a case of intramedullary SFT in the thoracic spine and review the literature.
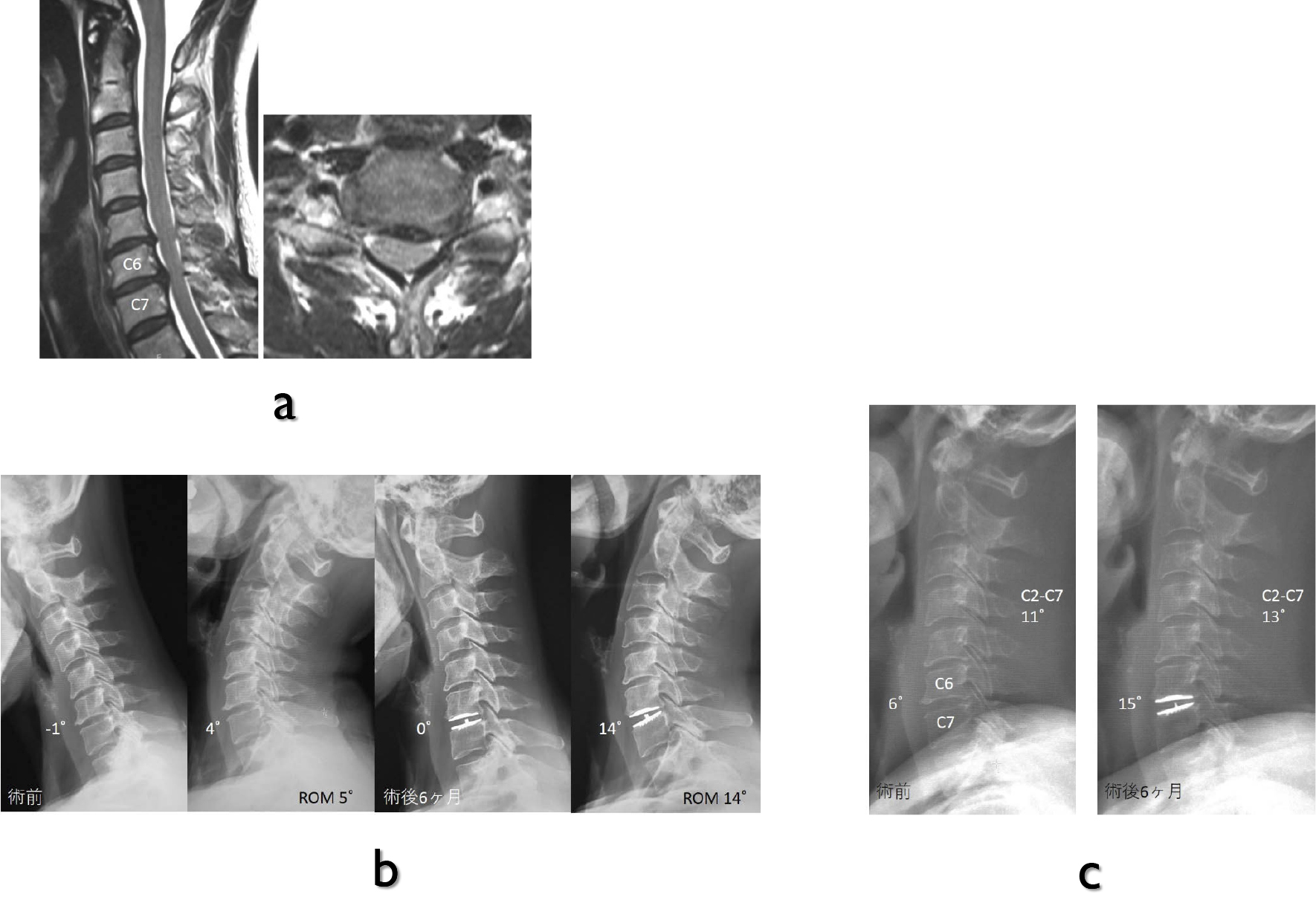
Case Report: A-47-year-old female complained gait disturbance and right lower leg numbness for 4 years. Intramedullary tumor was observed at Th2-Th3 level on MRI. The tumor showed isointensity on T1-weighted images, and hypointensity on T2-weighted images. It was homogeneously enhanced by gadolinium. Tumor resection with Th1-Th3 laminectomy was performed. Histopathological findings showed spindle-shaped cells proliferated irregularly with collagen fibers. Immunohistochemical staining revealed CD34 positive, and EMA, S-100 protein and GFAP were negative, so the diagnosis was SFT. After 3 months, she can walk without any aid. Six months after surgery, MRI showed no obvious recurrence of SFT.
Discussion: SFT is a mesenchymal tumor that was first reported as a localized pleural tumor in 1931, and was later reported to occur systemically. Since 1996, 41 cases of SFTs occurring in the spinal canal have been reported, and we analyzed these papers. The male-female ratio was 1.28:1 and the average age of onset was 51.1 years (17-83 years). Tumors occurred in 34.1% at the cervical level, 61.0% in the thoracic level, and 9.8% in the lumbar level. Tumor localization was 22.2% epidural, 33.3% intradural-extramedullary, and 36.1% intramedullary. On MRI findings, 78.6% of cases showed iso to hypo-intensity on T1-weighted images and iso to hypo-intensity on T2-weighted images. In gadolinium imaging, 80% were homogeneously contrasted. Immunohistochemical staining of SFTs shows positive for CD34 and negative for S-100 protein, GFAP, EMA, SMA and desmin. Differential diagnosis includes astrocytoma, ependymoma, hemangioblastoma, meningioma and schwannoma. A malignant case of SFTs occurring in the central nervous system is reported to be 5.8%, It has been reported that the recurrence rate of spinal SFTs was 14.8% in the case of total surgical removal and 80% in the case of partial removal.
Conclusion: We reported a rare case of SFT arise from spinal cord. Diagnosis should be done using MRI. Although most cases of SFTs are benign, recurrence cases and malignant cases have been also reported. Therefore, surgical total resection and careful long-term follow-up are important in treating SFTs of the spine.
View full abstract